A receding hairline or thinning crown drastically alters facial framing and overall aesthetic balance. Addressing progressive male pattern baldness requires precise surgical intervention rather than superficial cosmetic fixes. Undergoing a hair transplant in Turkey has emerged as the premier global solution, combining elite surgical expertise with highly advanced follicular extraction technologies. The clinical assessment of a successful procedure relies on meticulous visual inspection, evaluating everything from individual graft placement to the overarching density profile across the scalp.
Achieving a seamless, undetectable hairline restoration is the ultimate metric of surgical success. During a post-operative evaluation, dermatologists and restoration specialists analyze the integration of transplanted follicles with native hair. Through careful physical examination of the scalp, medical professionals can determine the exact survival rate of the grafts and the structural integrity of the newly established hairline. This comprehensive guide details the critical factors that contribute to optimal hair restoration outcomes and explores the advanced methodologies driving modern hair transplant procedures.
Video Chapters
- Assessing Natural Frontal Hairline Restoration Density
- Graft Placement and Natural Hair Growth Direction
- FUE Hair Transplant Versus DHI Techniques
- Addressing Severe Male Pattern Baldness
- Maximizing the Hair Graft Survival Rate
- Cost Benefits of Hair Loss Treatment Abroad
- Selecting Certified Medical Professionals
- Long-Term Post-Surgery Hair Maintenance
Assessing Natural Frontal Hairline Restoration Density
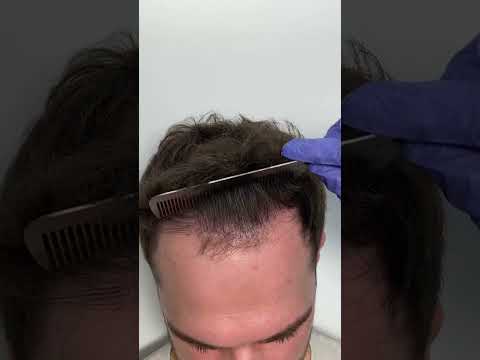
The creation of a biologically accurate frontal hairline represents the most challenging aspect of surgical hair restoration. Surgeons must carefully map the anterior boundary of the scalp, ensuring the design complements the patient's underlying facial structure and age-appropriate recession parameters. As demonstrated at [00:05], clinical evaluation involves parting the hair with a fine-toothed comb to expose the scalp. This technique allows medical professionals to assess the number of follicular units per square centimeter, verifying that the density matches the original biological growth pattern.
Natural hair does not grow in a perfectly straight, uniform line. Instead, it features micro-irregularities and a transition zone composed entirely of single-hair follicles. When evaluating a high-quality hair transplant in Turkey, these micro-irregularities serve as the hallmark of elite surgical craftsmanship. Placing double or triple-hair grafts directly on the leading edge of the hairline results in a harsh, artificial appearance often referred to as a "doll's hair" look. Experienced surgeons utilize ultra-fine punches and meticulously sort grafts under a microscope to prevent this outcome.
Beyond the initial transition zone, the density must gradually increase as it moves toward the mid-scalp. This gradient approach creates the illusion of profound thickness without depleting the limited donor supply at the back of the head. Achieving optimal frontal hairline restoration density requires an intricate balance of mathematics and artistry. The physician must calculate exactly how many grafts are required to block light from reflecting off the scalp, which is the primary visual cue for hair thinning.
The Importance of Graft Placement and Natural Hair Growth Direction
Density alone cannot produce a successful hair transplant; the precise angle and direction of each implanted follicle dictate the final aesthetic result. Native hair grows at distinct angles depending on its specific location on the scalp. At [00:10], parting the strands reveals how transplanted hair should seamlessly follow the native directional flow. In the frontal region, hair typically emerges at a forward-facing, acute angle of 15 to 30 degrees.
If a surgeon creates recipient sites at an incorrect angle, the resulting hair will stand straight up or cross over adjacent hairs, completely destroying the natural appearance. The use of specialized tools, such as sapphire blades, allows for the creation of incredibly precise recipient sites. These microscopically sharp instruments minimize tissue trauma while allowing the surgeon to dictate the exact depth and trajectory of the subsequent graft placement. This meticulous control is a primary reason why seeking an advanced hair transplant procedure yields superior cosmetic results.
The structural integrity of the recipient site directly influences the survival and behavior of the follicle. Coronal (lateral) slit techniques are frequently employed to ensure that the implanted graft lies flat against the scalp. This technique mimics the natural overlapping effect of human hair, known as shingling. By layering the hair properly, surgeons maximize visual coverage while efficiently utilizing the available donor follicles. Patients undergoing evaluations post-surgery look for this specific layering effect to confirm the procedure's success.
Evaluating FUE Hair Transplant in Turkey Versus DHI Techniques
Patients researching global hair restoration options inevitably encounter two primary methodologies: Follicular Unit Extraction (FUE) and Direct Hair Implantation (DHI). While both techniques utilize the same extraction protocols—harvesting individual grafts from the safe donor area at the back of the scalp—they differ significantly in the implantation phase. Understanding these differences is vital for patients selecting the most appropriate intervention for their specific pattern of alopecia.
| Surgical Feature | Sapphire FUE Technique | DHI (Direct Hair Implantation) |
|---|---|---|
| Implantation Method | Requires pre-made incisions using sapphire blades before forceps placement. | Simultaneous incision and placement using a specialized Choi Implanter Pen. |
| Shaving Requirement | Usually requires a full shave of the recipient area for optimal visibility. | Allows for unshaven hair transplants, ideal for placing grafts between existing hair. |
| Ideal Candidate | Patients requiring massive graft counts (3000+) for large bald areas. | Patients needing targeted density increases without fully cutting their hair. |
The Sapphire FUE method allows surgical teams to operate efficiently, making it the preferred choice for extensive balding patterns. Because the incisions are made in advance, technicians can rapidly place the grafts, minimizing the time the tissue spends outside the body. Conversely, the DHI method provides unparalleled protection for the follicle during insertion. The Choi pen shields the graft from mechanical trauma, potentially increasing the overall graft survival rate. Clinics specializing in hair transplant in Turkey generally offer both methodologies, tailoring the approach to the patient's precise anatomical needs.
Addressing Male Pattern Baldness with Advanced Follicular Extraction
Androgenetic alopecia, commonly known as male pattern baldness, is driven by genetic sensitivity to Dihydrotestosterone (DHT). This hormone binds to receptors in susceptible hair follicles, causing them to miniaturize, weaken, and eventually cease production. Because follicles situated in the occipital region (the back of the head) lack these specific DHT receptors, they remain structurally immune to the hormone's miniaturizing effects. Advanced follicular extraction leverages this biological loophole by relocating these DHT-resistant follicles to the bald regions.
Careful visual examinations, such as the one seen at [00:15], evaluate how well these extracted follicles establish themselves in DHT-affected zones. Proper integration requires healthy vascularization. Once the extracted graft is securely implanted into the recipient site, new blood vessels must form around the base of the follicle to supply oxygen and vital nutrients. This process, known as neovascularization, is critical during the first seventy-two hours post-operation.
Surgeons must carefully manage the extraction phase to avoid over-harvesting. Depleting the donor area can lead to a moth-eaten appearance, creating a secondary cosmetic issue that is notoriously difficult to repair. A highly skilled physician utilizes a randomized extraction pattern, taking no more than one out of every four consecutive follicles. This meticulous harvesting ensures that the donor region retains a naturally dense appearance even when worn very short.
Post-Operative Care Strategies for Maximum Hair Graft Survival Rate
The success of a hair restoration procedure is not solely dependent on the surgeon's skill in the operating room. Patient adherence to strict post-operative protocols drastically influences the final hair graft survival rate. In the immediate aftermath of the surgery, the newly implanted grafts are highly vulnerable to physical dislodgement and localized infection. Patients are instructed to sleep in a semi-upright position for the first five nights to minimize swelling and prevent accidental friction against pillows.
- Immediate Post-Op (Days 1-3): Focus on minimizing inflammation. Saline sprays are frequently used to keep the recipient area hydrated and promote rapid healing without disturbing the delicate grafts.
- Scab Removal (Days 4-10): Gentle washing techniques utilizing specialized foam shampoos help soften and remove crusts. Aggressive rubbing must be avoided to prevent extracting the anchored follicle.
- Shock Loss Phase (Weeks 3-6): The transplanted hair shafts shed due to surgical trauma. This is a normal physiological response; the root remains securely embedded and resting beneath the scalp.
- Growth Maturation (Months 6-12): New, permanent hair shafts emerge, initially fine and wispy, before thickening and texturizing to match the surrounding native hair characteristics.
Avoiding direct ultraviolet exposure, refraining from strenuous cardiovascular activity, and abstaining from alcohol and tobacco consumption are paramount during the critical healing window. Nicotine acts as a severe vasoconstrictor, limiting blood flow to the scalp and starving the new grafts of essential oxygen. Clinics specializing in hair transplant in Turkey provide extensive aftercare kits and continuous remote monitoring to ensure patients navigate the recovery timeline flawlessly.
Comprehensive Cost Benefits of Seeking Hair Loss Treatment Abroad
The financial dynamics of medical procedures have shifted significantly, driving thousands of patients to seek cross-border healthcare solutions. The cost of a premium hair restoration surgery in North America or Western Europe can easily exceed traditional budgetary constraints. In contrast, securing a high-quality hair transplant in Turkey offers profound financial advantages without compromising clinical standards. The price disparity is largely driven by differences in overhead costs, localized labor rates, and currency exchange valuations.
International patients benefit from structured, all-inclusive medical packages. These comprehensive itineraries typically cover the full cost of the surgical procedure, required pre-operative blood panels, VIP airport transfers, and luxury hotel accommodations near the clinic. By consolidating these logistical elements, the stress associated with medical travel is entirely neutralized. Patients can focus solely on their physical recovery and immediate post-operative instructions.
However, cost should never serve as the sole determining factor when pursuing invasive cosmetic procedures. The true value of seeking hair loss treatment abroad lies in accessing highly specialized medical teams who perform these specific surgeries daily. A dedicated hair transplant surgeon operating in a premier global hub accumulates vast clinical experience rapidly, encountering every conceivable hair type, skin laxity variation, and balding pattern. This concentrated expertise directly translates to superior aesthetic outcomes and minimized complication rates.
Selecting Certified Medical Professionals for Hair Restoration
The proliferation of international medical tourism has necessitated rigorous vetting processes for prospective patients. Selecting the right clinic requires verifying the credentials of the operating physician. Patients must prioritize clinics led by doctors affiliated with recognized global medical boards, such as the International Society of Hair Restoration Surgery (ISHRS). This certification ensures that the clinic adheres to standardized, ethical medical practices and utilizes sterilized, state-of-the-art clinical environments.
A critical aspect of clinical evaluation is reviewing high-definition, unedited macroscopic footage of previous patients. Detailed physical checks, like the examination occurring at [00:20], provide tangible proof of a clinic's capability. Prospective patients should look closely for proper donor site healing, lack of visible scarring, and natural structural blending in the recipient area. Clinics that rely heavily on uncertified technicians to perform the critical extraction and incision phases should be strictly avoided.
During the initial consultation, a qualified physician will provide a highly individualized assessment rather than a generic sales pitch. They will measure the exact surface area requiring coverage using specialized densitometers and transparent grid tools. The doctor must provide a realistic projection of what can be achieved in a single surgical session. If a patient possesses severe Norwood Class VI or VII baldness with limited donor reserves, an ethical professional will outline a multi-stage approach or clearly advise against surgery entirely.
Long-Term Maintenance and Medical Therapies Post-Surgery
A hair transplant effectively redistributes existing hair; it does not cure the underlying genetic predisposition to hair loss. The native, non-transplanted hair residing on the top of the scalp remains susceptible to the miniaturizing effects of DHT. Without proactive, long-term maintenance, patients risk developing unnatural gaps behind their newly transplanted frontal hairline as their native hair continues to shed. A comprehensive medical management plan is strictly required to preserve the surrounding follicular units.
Physicians routinely prescribe FDA-approved medical therapies to stabilize progressive shedding. Oral 5-alpha reductase inhibitors block the conversion of testosterone into DHT, shielding the vulnerable native hair. Topical vasodilators are also utilized to prolong the anagen (growth) phase of the hair cycle and increase blood circulation directly at the scalp level. As seen in final structural comb-throughs at [00:25], the density is maintained heavily through the synergy of surgery and ongoing medical intervention.
In addition to conventional pharmaceuticals, adjuvant therapies have gained significant traction in postoperative protocols. Platelet-Rich Plasma (PRP) treatments involve drawing the patient's blood, isolating the concentrated growth factors in a centrifuge, and injecting the plasma directly into the scalp. PRP therapies accelerate tissue healing immediately following the FUE hair transplant and continuously stimulate dormant follicles. Integrating these advanced clinical maintenance strategies ensures the surgical results remain robust, dense, and visually flawless for decades.
Secure Your Custom Hair Restoration Assessment
Take the decisive step toward reclaiming a natural, dense hairline. Connect directly with board-certified medical teams globally to receive a comprehensive evaluation of your hair loss condition and a detailed procedure plan.
Get Free QuoteView Full Video Transcript & Clinical Timeline
00:00 - Initial visual assessment begins, highlighting the established density across the frontal scalp and structural integrity of the grafted follicles.
00:05 - Medical practitioner utilizes a fine-tooth comb to part the mid-scalp hair, revealing excellent root density and the absence of scarring.
00:10 - The comb moves laterally across the left temporal peak, demonstrating proper angulation and natural forward growth direction of the implanted hair.
00:15 - Closer evaluation of the central forelock region; the transition zone shows precise placement of single-hair grafts to avoid an artificial baseline.
00:20 - Right temporal region parted; the native hair blends flawlessly with the transplanted units, showcasing a seamless gradient and strong structural support.
00:25 - Final comb-through toward the vertex. The scalp coverage successfully blocks light reflection, confirming high graft survival rates.
00:30 - Conclusion of the clinical evaluation; hair is styled forward to demonstrate real-world cosmetic impact and functional density.















Share this listing