The Complete Guide to Gastric Sleeve Surgery: Live Bariatric Procedure by Assoc. Prof. Dr. Cemal Kara
Struggling with severe obesity often feels like an unwinnable battle against your own biology, where traditional diets and exercise regimens continuously fall short. Today, advanced bariatric surgery offers a scientifically proven, permanent pathway to reclaiming your health, mobility, and lifespan. This detailed breakdown explores a live gastric sleeve weight loss surgery performed by the esteemed Assoc. Prof. Dr. Cemal Kara.
By watching the precise techniques involved in laparoscopic sleeve gastrectomy, patients can demystify the operating room experience. Understanding the surgical process is the first critical step toward overcoming pre-operative anxiety. Explore exactly how this minimally invasive stomach reduction surgery alters metabolic function, restricts caloric intake, and sets the stage for massive, sustainable weight loss.
Video Chapters & Quick Navigation
- Understanding Laparoscopic Gastric Sleeve
- Patient Preparation & Assessment
- Surgical Setup & Anesthesia
- Step-by-Step Live Procedure
- Dr. Cemal Kara's Expertise
- Post-Operative Recovery Timeline
- Post-Bariatric Nutritional Guidelines
- Expected Metabolic Benefits
- Managing Potential Risks
- Bariatric Medical Tourism Options
Understanding Laparoscopic Gastric Sleeve Surgery
Laparoscopic sleeve gastrectomy, widely known as gastric sleeve surgery, is currently the most popular bariatric procedure performed worldwide. It involves the surgical removal of approximately 75% to 80% of the stomach, leaving behind a narrow, banana-shaped "sleeve" or tube. This massive reduction in stomach volume fundamentally alters how a patient consumes and processes food.
Unlike older, more invasive open surgeries, the laparoscopic approach utilizes tiny incisions, a specialized camera, and long surgical instruments. This minimally invasive technique significantly reduces post-operative pain and dramatically shortens the hospital stay. Furthermore, the risk of massive surgical scarring or incisional hernias is greatly minimized.
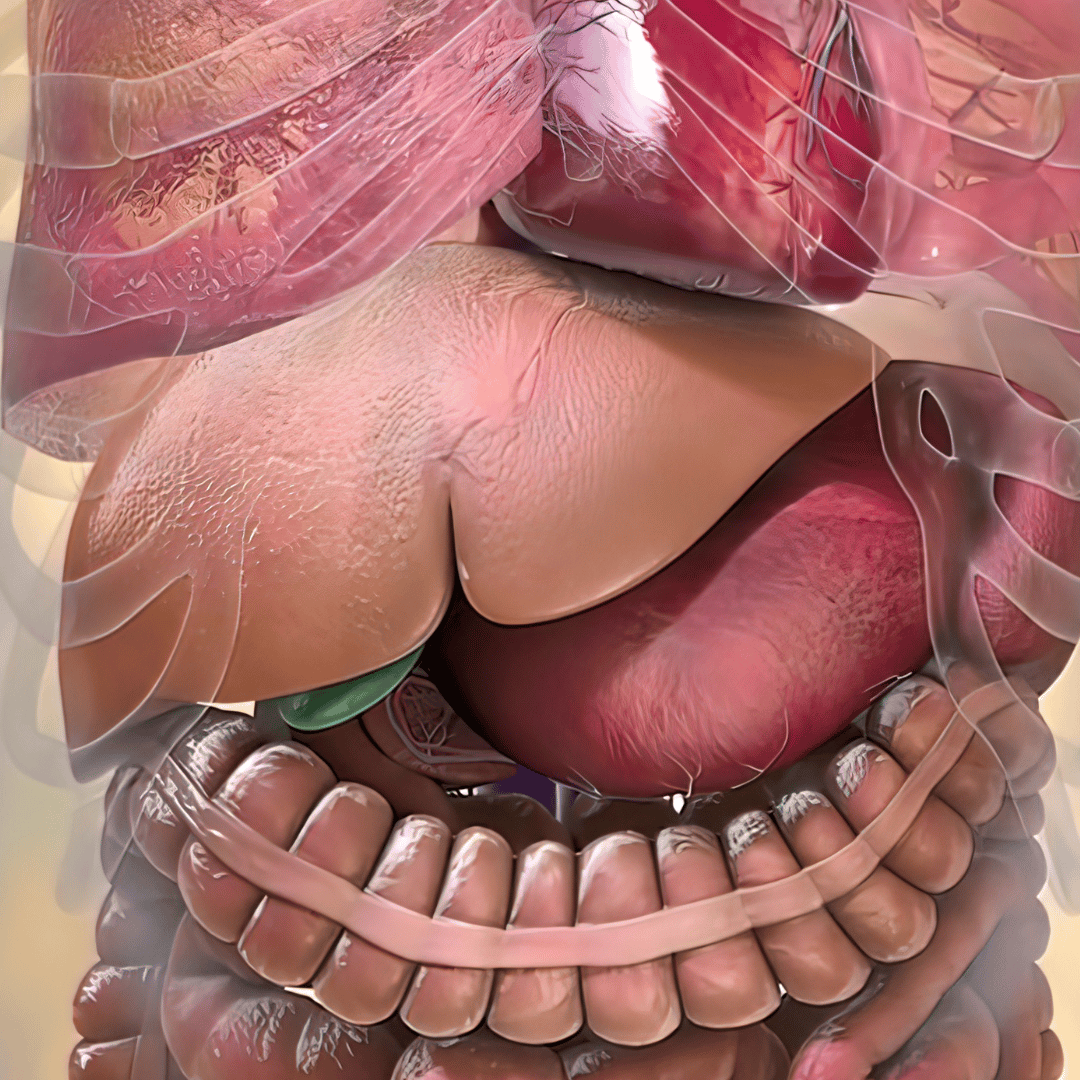
Beyond simple caloric restriction, the removal of the stomach's fundus creates a profound metabolic shift. The fundus is the primary production site for ghrelin, the hormone responsible for signaling hunger to the brain. By excising this tissue, patients experience a massive reduction in physiological cravings, making post-operative dietary adherence far more manageable.
Patient Preparation and Pre-Operative Assessment
Success in bariatric surgery begins long before the patient ever enters the operating room. A comprehensive pre-operative assessment is mandatory to ensure the patient is physically and psychologically ready for a massive lifestyle transformation. This typically involves blood work, cardiovascular stress testing, and a thorough psychological evaluation.
Patients are often placed on a specialized pre-operative liver-shrinking diet starting one to two weeks before the surgery. Because the liver sits directly over the stomach, a fatty or enlarged liver can severely obstruct the surgeon's view during a laparoscopic procedure. This low-carbohydrate, low-calorie diet forces the body to burn glycogen stores, effectively shrinking the liver and making the operation safer.
In addition to dietary changes, patients are required to cease smoking and discontinue certain blood-thinning medications well in advance. Smoking severely impairs tissue healing and increases the risk of post-operative leaks at the staple line. Surgeons like Assoc. Prof. Dr. Cemal Kara strictly enforce these guidelines to guarantee the highest safety standards for obesity treatment options.
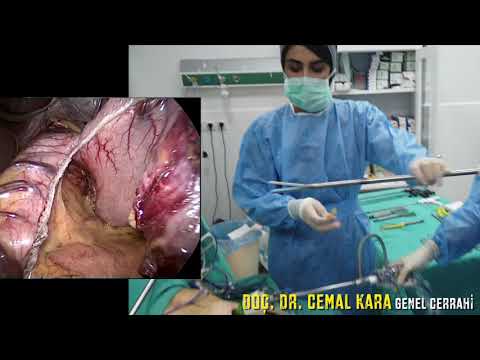
Surgical Room Setup and Anesthesia Protocols
As seen at in the live broadcast, the surgical room setup for a bariatric procedure is highly specialized. The patient is placed under general anesthesia to ensure complete unconsciousness and muscle relaxation throughout the procedure. Advanced monitoring equipment tracks the patient's heart rate, oxygen saturation, and blood pressure in real-time.
The patient is carefully positioned on the operating table, often in a steep reverse Trendelenburg position (head up, feet down). This specific angle utilizes gravity to pull the intestines and surrounding organs downward, providing the surgeon with a clear, unobstructed view of the upper abdomen and stomach. Safety straps and specialized padding are used to prevent nerve damage or pressure sores during this positioning.
Once the patient is prepped and draped, the surgical team performs a final "time-out" to verify patient identity, surgical consent, and equipment readiness. This global safety standard prevents errors and ensures that all high-tech laparoscopic tools, including the harmonic scalpel and endoscopic staplers, are fully functional before the first incision is made.
Step-by-Step Live Gastric Sleeve Procedure Breakdown
The core of this educational video provides an unprecedented, over-the-shoulder look at the exact mechanics of a stomach reduction surgery. Assoc. Prof. Dr. Cemal Kara demonstrates absolute precision, executing each phase of the operation with practiced efficiency. Breaking down these steps helps demystify the complex medical terminology.
Trocar Placement and Abdominal Access
The surgery begins at with the creation of pneumoperitoneum. Dr. Kara inflates the abdominal cavity with harmless carbon dioxide gas, creating a spacious working dome. This inflation is critical as it separates the abdominal wall from the internal organs, preventing accidental injury during instrument insertion.
Following inflation, several small incisions (typically 4 to 5) are made to insert cylindrical ports called trocars. The high-definition laparoscope is inserted through one trocar, broadcasting a magnified, highly detailed view of the stomach to the surgical monitors. The remaining trocars serve as pathways for the specialized, long-handled surgical instruments.
Stomach Mobilization and Blood Vessel Ligation
Before the stomach can be divided, it must be freed from its surrounding attachments. At , Dr. Kara uses an advanced ultrasonic energy device to dissect the greater curvature of the stomach. This tool simultaneously cuts tissue and seals blood vessels, drastically minimizing blood loss.
The surgeon carefully detaches the greater omentum and ligates the short gastric vessels that connect the stomach to the spleen. This is a delicate process requiring immense skill, as the spleen is a highly vascular organ prone to bleeding if disturbed. Complete mobilization ensures the stomach can be stretched out cleanly for a straight, uniform staple line.
Stomach Resection with Endoscopic Staplers
The defining moment of the gastric sleeve weight loss surgery occurs around . An anesthesiologist passes a sizing tube, known as a bougie, down the patient's esophagus and into the stomach. This tube acts as a physical template, ensuring the new stomach sleeve is perfectly sized—neither too narrow to cause strictures nor too wide to compromise weight loss.
Dr. Kara then introduces a specialized endoscopic stapler. Starting from the lower portion of the stomach (the antrum) and moving upward toward the esophagus, the stapler sequentially fires titanium staples while simultaneously cutting the tissue. The large, excised portion of the stomach is entirely separated and eventually removed from the abdomen through one of the slightly enlarged trocar incisions.
Leak Testing and Final Inspection
Patient safety is paramount, making the leak test at one of the most critical steps of the procedure. The surgical team typically injects a blue dye (methylene blue) or air through the bougie into the new stomach pouch. Dr. Kara closely inspects the entire staple line under the camera to ensure there is no bubbling or dye leakage.
Once the staple line is confirmed to be completely secure, the trocars are carefully withdrawn. The small abdominal incisions are then closed using dissolvable sutures or surgical glue. The entire live procedure typically takes less than an hour in the hands of an experienced bariatric specialist.
The Role of Assoc. Prof. Dr. Cemal Kara in Bariatric Innovations
Observing Assoc. Prof. Dr. Cemal Kara during this live broadcast highlights the immense value of surgical experience. Bariatric surgery is not merely a mechanical process; it requires deep anatomical knowledge and the ability to adapt instantly to patient-specific variations. Dr. Kara's methodical approach reflects years of specialized training in advanced metabolic surgery.
Surgeons of his caliber contribute significantly to the evolution of high volume long-tail bariatric procedures. By participating in live demonstrations and sharing surgical outcomes, Dr. Kara helps standardize best practices across the global medical community. This transparency builds immense trust with prospective patients seeking obesity treatment options.
His use of advanced staple line reinforcement techniques and meticulous tissue handling directly translates to lower complication rates and faster patient recovery. Choosing a highly credentialed, board-certified bariatric surgeon is the single most important decision a patient can make to ensure long-term weight loss maintenance and surgical safety.
Post-Operative Care and The Recovery Timeline
Immediately following the bariatric surgery live procedure, the patient is moved to the recovery ward for close observation. Pain is generally well-managed with intravenous medications, and patients are actively encouraged to stand up and walk within hours of waking up. Early mobilization is a vital protocol to prevent deep vein thrombosis (blood clots) and encourage respiratory function.
The hospital stay for a laparoscopic sleeve gastrectomy is remarkably short, usually lasting only one to two nights. During this time, the medical team monitors hydration levels, ensures the patient can tolerate sips of water, and watches for any early signs of infection. Most patients report feeling fatigue rather than severe pain.
The complete bariatric surgery recovery time spans several weeks. Patients usually return to desk work within 10 to 14 days, though strenuous physical lifting must be avoided for at least four to six weeks. Adhering strictly to the surgeon's post-operative guidelines is crucial during this delicate healing phase.
Nutritional Guidelines After Bariatric Surgery
The physical surgery is only half of the journey; the other half relies entirely on radical dietary modifications. Because the new stomach sleeve holds merely 3 to 4 ounces of food, patients must relearn how to eat, drink, and process nutrition. A phased dietary approach is implemented to allow the staple line to heal without stretching or tearing.
Patients start on a strict clear liquid diet for the first week, consuming broths, sugar-free popsicles, and diluted juices. This transitions into full liquids and protein shakes, emphasizing high-protein intake to promote tissue healing and prevent muscle loss. Hydration is challenging due to the small stomach capacity, requiring patients to sip water constantly throughout the day.
| Dietary Phase | Timeline | Permitted Foods |
|---|---|---|
| Phase 1: Clear Liquids | Days 1 - 7 | Water, clear broth, sugar-free gelatin, decaf tea. |
| Phase 2: Full Liquids | Days 8 - 14 | Protein shakes, skim milk, strained cream soups. |
| Phase 3: Pureed Foods | Weeks 3 - 4 | Blended meats, scrambled eggs, cottage cheese, hummus. |
| Phase 4: Soft Foods | Weeks 5 - 6 | Flaky fish, soft vegetables, ground lean turkey. |
| Phase 5: Stabilization | Week 7+ | Solid healthy foods. Focus on protein first, small portions. |
Expected Weight Loss Outcomes and Metabolic Benefits
The primary motivation for undergoing a gastric sleeve weight loss surgery is the dramatic, sustained reduction in body weight. On average, patients can expect to lose 60% to 70% of their excess body weight within the first 12 to 18 months post-operation. The most rapid weight loss typically occurs during the first six months.
However, the benefits of metabolic surgery extend far beyond the numbers on a scale. Bariatric surgery is highly effective in treating, and often completely resolving, obesity-related comorbidities. Patients frequently experience complete remission of Type 2 diabetes, drastic improvements in obstructive sleep apnea, and a significant lowering of high blood pressure.
Furthermore, the reduction in joint pressure severely decreases the symptoms of osteoarthritis, granting patients newfound mobility. The psychological benefits are equally profound, with patients reporting massive improvements in self-esteem, reduced rates of depression, and a massively enhanced overall quality of life.
Potential Risks and Long-Term Complication Management
While the laparoscopic sleeve gastrectomy is considered incredibly safe, it remains a major surgical intervention with inherent risks. Short-term risks include bleeding, infection, or the highly dangerous staple line leak. A staple line leak occurs when digestive fluids escape the stomach pouch into the abdominal cavity, requiring immediate emergency medical intervention.
Long-term considerations involve nutritional deficiencies and gastrointestinal changes. Because the stomach capacity is severely reduced, patients are required to take specialized bariatric multivitamins, calcium, and B12 supplements for the rest of their lives. Failure to adhere to supplementation can lead to anemia, osteoporosis, or severe neurological issues.
Another common long-term side effect is the development or worsening of gastroesophageal reflux disease (GERD). Because the stomach tube is high-pressure, acid can be forced upwards into the esophagus. If severe GERD develops and remains unresponsive to medication, a revision surgery to a gastric bypass may be necessary to correct the issue.
Why Choose Medical Tourism for Bariatric Surgery?
In regions like the United States, the United Kingdom, and Canada, bariatric surgery can be prohibitively expensive, often costing upwards of $15,000 to $25,000 out of pocket. Furthermore, stringent insurance requirements and prolonged public health waiting lists can delay life-saving treatment for years. This frustration has driven a massive surge in medical tourism for obesity treatment options.
Countries like Turkey have emerged as global hubs for bariatric excellence, offering world-class facilities and internationally board-certified surgeons like Assoc. Prof. Dr. Cemal Kara. Patients traveling abroad can often secure comprehensive all-inclusive packages for a fraction of the domestic cost. These packages frequently include VIP airport transfers, luxury hotel accommodations, the surgery itself, and comprehensive pre-operative diagnostics.
Opting for bariatric medical tourism does not mean compromising on safety or quality. In fact, many international clinics utilize cutting-edge medical technology that meets or exceeds North American standards. By partnering with trusted medical tourism facilitators, patients can embark on a seamless, highly coordinated journey toward massive weight loss and renewed health.
Ready to Start Your Weight Loss Transformation?
Don't let high costs or long waiting lists delay your journey to a healthier, happier life. Connect with elite, board-certified bariatric surgeons globally and discover affordable, all-inclusive medical tourism packages tailored to your specific health needs.
REQUEST YOUR FREE BARIATRIC QUOTE

.png)






Share this listing