Shoulder Injury Treatment Success: Paula Acosta’s Stem Cell Therapy Experience in Santo Domingo, DR
Living with a debilitating joint issue can drain the joy from daily life, but Paula Acosta’s stem cell therapy experience in Santo Domingo, DR, highlights a revolutionary path to healing. When standard treatments fail, regenerative medicine offers profound hope for those suffering from chronic pain. This comprehensive guide explores how targeted orthopedic stem cell therapy abroad is transforming the way we treat severe joint degeneration. Discover why proactive patients are bypassing invasive surgeries, avoiding lengthy rehabilitation periods, and choosing medical tourism in the Dominican Republic for effective, non-surgical shoulder pain relief.
Video Chapters & Quick Navigation
The Devastating Impact of Chronic Shoulder Injuries
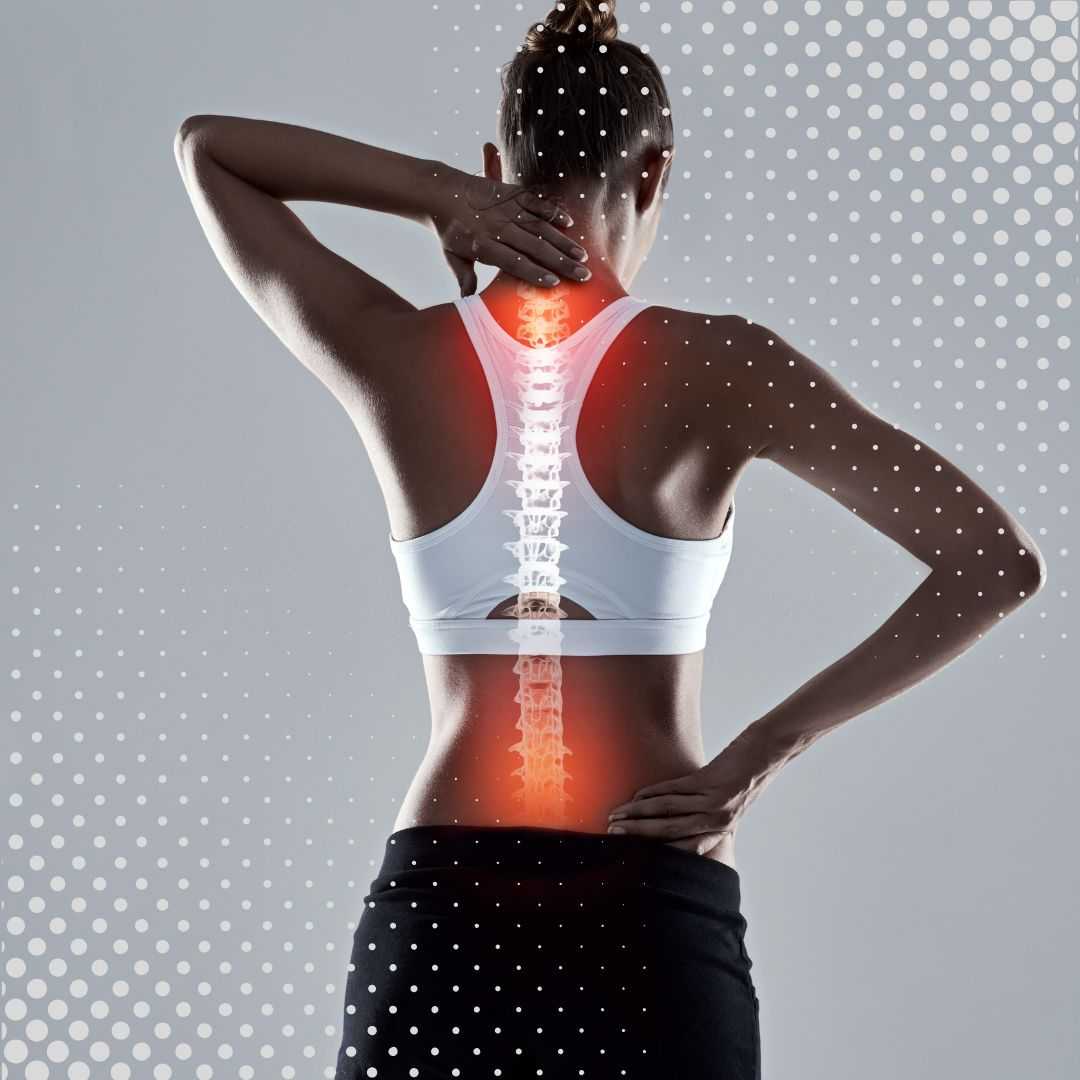
The human shoulder is an incredibly complex piece of biological machinery. Known anatomically as the glenohumeral joint, it boasts the greatest range of motion of any joint in the human body. This remarkable flexibility, however, comes at a high cost: a profound susceptibility to instability, wear and tear, and traumatic injury. For individuals suffering from chronic shoulder pain, everyday tasks such as reaching for a high shelf, putting on a jacket, or simply finding a comfortable sleeping position can become agonizing ordeals.
Common culprits include rotator cuff tears, osteoarthritis, bursitis, and labral tears. Over time, the protective cartilage that cushions the joint begins to degrade, leading to bone-on-bone friction. Furthermore, the tendons and ligaments that stabilize the shoulder can suffer micro-tears from repetitive motion or sports injuries. As Paula Acosta notes at in her video testimonial, the sheer exhaustion of living with relentless, radiating shoulder pain can take a massive psychological toll, completely upending an active lifestyle.
Unfortunately, the body's natural healing mechanisms are often insufficient when it comes to severe connective tissue damage. Tendons and cartilage have notoriously poor blood supply, meaning that once they are damaged, they struggle to repair themselves. This biological limitation is precisely why chronic shoulder injuries rarely resolve on their own, forcing patients to seek medical interventions that range from temporary pharmaceutical band-aids to invasive joint reconstruction.
Why Traditional Shoulder Surgery Isn't Always the Best Answer
For decades, the standard orthopedic protocol for a failing shoulder joint has followed a predictable, and often frustrating, trajectory. Patients are typically prescribed non-steroidal anti-inflammatory drugs (NSAIDs) and corticosteroid injections to manage the symptoms. While these may offer fleeting relief, clinical studies have repeatedly shown that repetitive steroid injections can actually accelerate cartilage degradation and weaken tendons over time. When these conservative measures inevitably fail, orthopedic surgeons will recommend arthroscopic repair or total joint replacement.
However, shoulder surgery is fraught with significant drawbacks. The procedure itself carries risks of infection, nerve damage, and anesthesia complications. Post-operatively, patients are usually subjected to a grueling rehabilitation process that can last anywhere from six to twelve months. During this time, the shoulder is largely immobilized, leading to muscle atrophy and a drastic reduction in quality of life. Furthermore, surgical interventions are not foolproof; a significant percentage of patients report persistent pain or stiffness even after a "successful" operation, leading to a search for alternatives around into their journey.
| Feature | Traditional Shoulder Surgery | Stem Cell Therapy |
|---|---|---|
| Invasiveness | Highly invasive, requires incisions and anesthesia | Minimally invasive, performed via ultrasound-guided injection |
| Recovery Time | 6 to 12 months of intense rehabilitation | Minimal downtime, often returning to light activities in weeks |
| Scarring | Visible external scarring, internal scar tissue formation | No surgical scarring |
| Primary Mechanism | Mechanical repair, removal of damaged tissue | Biological cellular regeneration and inflammation reduction |
Exploring Regenerative Medicine: How Stem Cell Therapy Works for Shoulders
The fundamental promise of regenerative medicine is to harness and amplify the body’s innate ability to heal itself. At the center of this medical revolution are Mesenchymal Stem Cells (MSCs). These are multipotent adult stem cells that have the unique ability to differentiate into various types of musculoskeletal tissues, including bone, cartilage, muscle, and tendon cells. When introduced into a damaged shoulder joint, they do not merely mask the pain; they actively work to repair the underlying structural deficit.
When high concentrations of MSCs are injected into an injured rotator cuff or arthritic shoulder capsule, they initiate a powerful cascade of healing events known as the paracrine effect. First, the stem cells act as highly intelligent biological managers, homing in on the exact sites of severe inflammation. They release potent anti-inflammatory cytokines that rapidly calm the hostile environment within the joint. This immediate reduction in inflammation is often responsible for the rapid pain relief many patients experience.
Following this initial phase, the stem cells begin to secrete growth factors that stimulate angiogenesis—the formation of new blood vessels. By restoring robust blood flow to the previously avascular regions of the shoulder tendons, the body can finally deliver the oxygen and nutrients required for cellular remodeling. The stem cells then encourage the patient’s own native cells to proliferate and lay down new, healthy collagen matrices, effectively patching micro-tears and rebuilding degraded cartilage from the inside out.
Paula Acosta's Journey: Seeking Alternative Treatment Abroad
Paula Acosta’s narrative is a textbook example of the modern patient’s dilemma. Facing a significant shoulder injury that severely limited her mobility, she was presented with the grim prospect of surgery. The thought of spending months in a sling, reliant on painkillers, and unable to work or participate in her favorite hobbies was entirely unappealing. She recognized that removing or mechanically altering the joint might solve one problem but create a host of others down the line.
Determined to find a better way, Paula began researching non-surgical alternatives to shoulder replacement and rotator cuff repair. Her extensive research into regenerative medicine led her to discover the profound benefits of stem cell therapy. However, she quickly encountered a major roadblock: accessing advanced, high-cell-count therapies in her home country was prohibitively expensive and strictly limited by domestic medical regulations. This pivotal realization, detailed at , prompted her to look beyond her borders and explore international medical tourism options.
Her search culminated in Santo Domingo, Dominican Republic. Here, she found top-tier medical facilities offering highly concentrated, ethically sourced mesenchymal stem cell treatments that adhere to rigorous international safety standards. By stepping outside her local healthcare system, Paula was able to access a level of regenerative care that completely changed the trajectory of her joint health.
Why Santo Domingo, Dominican Republic is a Hub for Stem Cell Therapy
The Dominican Republic has rapidly emerged as a premier destination for medical tourists seeking cutting-edge orthopedic treatments. But why Santo Domingo? The answer lies in a perfect convergence of advanced medical infrastructure, highly specialized physicians, geographic proximity to North America, and a more progressive regulatory environment for cellular therapies.
In many Western countries, such as the United States, regulatory bodies impose strict limitations on how stem cells can be processed and administered. Often, clinics are restricted to using minimally manipulated autologous cells (harvested from the patient’s own body on the same day), which yields a relatively low cell count, especially in older patients. In contrast, leading clinics in Santo Domingo operate under international protocols that allow for the safe, laboratory-controlled expansion of stem cells. This means patients can receive treatments containing tens of millions of potent, youthful MSCs—vastly increasing the regenerative potential of the injection.
Furthermore, the medical facilities in Santo Domingo are state-of-the-art. The regenerative medicine clinics boast sterile, high-tech laboratories and are staffed by bilingual, internationally board-certified orthopedic specialists and scientists. Patients traveling to the DR benefit not only from world-class medical expertise but also from the warm, healing environment of a Caribbean paradise, making the entire medical journey far less stressful than a sterile hospital visit back home.
The Stem Cell Procedure: What to Expect Step-by-Step
Understanding the clinical process is crucial for alleviating the anxiety associated with medical travel. As highlighted around in the video, the experience in Santo Domingo is designed to be seamless, highly personalized, and completely patient-centric. Here is an overview of the typical procedural steps for shoulder stem cell therapy:
- 1. Comprehensive Diagnostic Evaluation: The process begins with a thorough review of the patient's medical history, physical mobility tests, and high-resolution imaging (such as MRI or ultrasound) to pinpoint the exact location and severity of the tissue damage.
- 2. Cell Preparation and Culturing: Depending on the specific protocol, premium stem cells (often derived from ethically sourced, FDA-screened umbilical cord Wharton's Jelly) are prepared in a highly controlled laboratory setting to ensure maximum viability and concentration.
- 3. Precision Image-Guided Injection: This is the most critical step. Using advanced fluoroscopy or real-time ultrasound guidance, the specialized orthopedic physician delivers the concentrated stem cells directly into the micro-tears, joint capsule, or damaged cartilage with pinpoint accuracy.
- 4. Immediate Post-Care and Observation: The procedure is entirely outpatient. Following a brief observation period where joint mobility is checked and post-care instructions are provided, the patient is cleared to return to their hotel to begin the recovery process.
The Financial Advantage: Cost of Stem Cell Therapy for Shoulder Pain
It is impossible to discuss medical tourism without addressing the profound economic benefits. In North America and parts of Europe, regenerative treatments are rarely covered by standard health insurance policies, as they are often still classified as elective or experimental by insurance boards. Consequently, patients are forced to pay entirely out of pocket. A single orthopedic stem cell injection in the United States can easily cost between $6,000 and $12,000, and this often utilizes a lower concentration of cells due to domestic regulatory constraints on cell expansion.
By choosing to travel to Santo Domingo, patients can access significantly superior biologic treatments at a fraction of the cost. Comprehensive regenerative medicine packages in the Dominican Republic typically range from $3,500 to $6,000. These medical tourism packages frequently include not only the advanced stem cell injection itself but also pre-procedure consultations, ground transportation, concierge services, and sometimes even luxury hotel accommodations.
When you factor in the indirect costs of traditional surgery—such as months of lost wages due to time off work, expensive post-operative physical therapy copays, and the price of prescription pain medications—the financial logic of seeking non-surgical stem cell therapy abroad becomes overwhelmingly clear. It is a cost-effective investment in long-term joint health and rapid functional restoration.
Life After Regenerative Treatment: Paula’s Recovery Timeline
One of the most appealing aspects of Paula's story, highlighted near , is the stark contrast between her rapid recovery and the grueling rehabilitation required after traditional shoulder surgery. Because stem cell therapy is minimally invasive, it does not inflict secondary trauma on the body. There are no muscles to cut through, no bones to drill, and no hardware to install.
The immediate aftermath of the injection usually involves mild soreness and swelling at the injection site. This is actually a positive sign; it indicates that the stem cells have successfully triggered the acute, localized inflammatory response necessary to kickstart the healing cascade. Patients are generally advised to rest the joint for the first 48 to 72 hours, avoiding any heavy lifting or strenuous overhead movements.
Between weeks two and six, the biological magic truly begins. The stem cells actively proliferate, signaling the body to lay down new collagen fibers and repair damaged tissue. During this phase, patients typically report a significant and steady decrease in their chronic pain levels, coupled with a gradual return of range of motion. By months three to six, the remodeling phase is well underway. The newly formed tissue matures and strengthens, allowing patients to confidently return to the sports, hobbies, and daily activities that their shoulder injuries had previously stolen from them.
Maximizing the Success of Your Orthopedic Stem Cell Treatment
While the regenerative power of stem cells is remarkable, the ultimate success of the therapy relies heavily on the patient's commitment to post-procedure care. To ensure the newly injected cells survive, thrive, and integrate effectively into the shoulder joint, specific biochemical and biomechanical environments must be maintained.
Crucially, patients must strictly avoid Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) like ibuprofen or naproxen for several weeks before and after the procedure. As counterintuitive as it may seem, the localized inflammation generated immediately after the injection is the exact signaling mechanism the stem cells use to determine where to heal. Suppressing this signal with medication can severely blunt the efficacy of the entire treatment.
Furthermore, integrating targeted physical therapy is vital. As discussed at , while you avoid the heavy rehab of surgery, gentle, guided movements are necessary. Proper physical therapy helps align the new collagen fibers along the natural lines of physical stress, ensuring that the repaired tendon or cartilage is both strong and flexible. Coupled with a nutrient-rich, anti-inflammatory diet to support cellular health, patients like Paula Acosta can achieve complete, long-lasting restoration of their shoulder function.
Ready to Overcome Shoulder Pain Without Surgery?
Stop letting chronic joint pain dictate your life. Connect with world-class regenerative medicine specialists in Santo Domingo, DR. Discover if advanced stem cell therapy is the right solution to repair your shoulder and restore your active lifestyle.
GET A FREE CONSULTATION & QUOTE

.png)




.png)






Share this listing