Patients dealing with debilitating nerve compression are increasingly seeking advanced robotic spinal stenosis surgery in Turkey to achieve long-lasting pain relief. Degenerative spine conditions often create progressive symptoms that severely limit daily mobility and overall quality of life. Exploring international healthcare options has become a primary strategy for individuals requiring complex orthopedic interventions without enduring excessive wait times.
Choosing to undergo a major orthopedic procedure abroad involves careful consideration of medical technology, surgical expertise, and post-operative rehabilitation protocols. By utilizing state-of-the-art robotic assistance, specialized orthopedic clinics can offer unprecedented precision during spinal decompression and fusion procedures. This detailed analysis examines the clinical pathways, technological advantages, and patient experiences associated with international spine care.
Video Chapters & Quick Navigation
- Understanding Degenerative Spinal Stenosis Progression
- Clinical Assessment and Surgical Consultation Protocols
- Technological Superiority of Robotic-Assisted Spine Surgery
- Accelerated Post-Operative Recovery and Mobilization
- Strategic Advantages of Medical Tourism for Orthopedics
- Criteria for Selecting High-Authority International Clinics
- Comprehensive Risk Management in Complex Spine Interventions
- Logistical Preparation for Cross-Border Healthcare Journeys
Understanding Degenerative Spinal Stenosis Progression and Chronic Pain
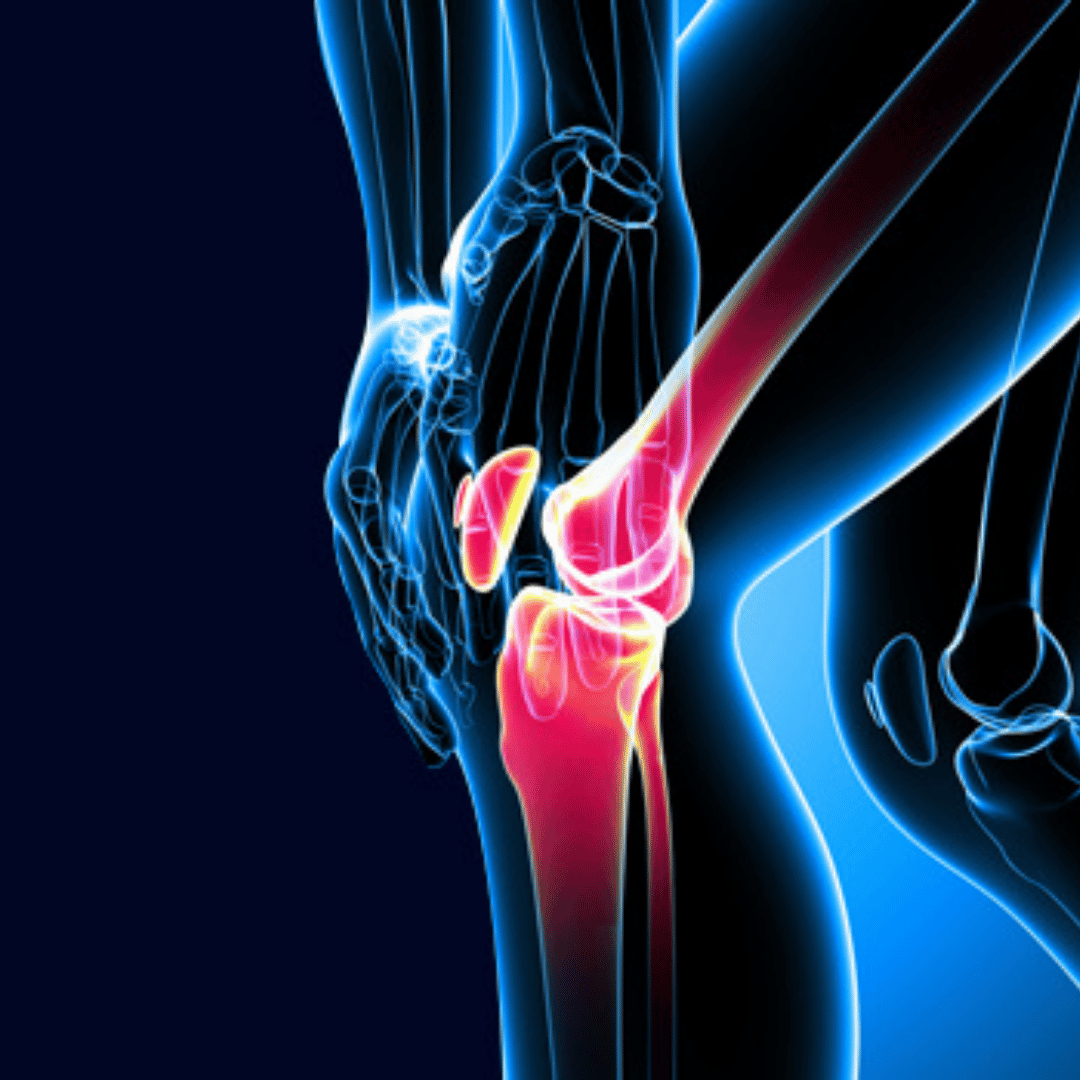
The clinical manifestation of degenerative spinal stenosis is characterized by a gradual narrowing of the spaces within the spine. This anatomical constriction places severe pressure on the spinal cord and the traversing nerve roots. As documented in early clinical assessments around [00:00], patients frequently report that back pain symptoms start as mild discomfort before progressing aggressively. Over time, the structural degradation within the lumbar region compromises the body's primary neurological pathways.
In a standard timeline of spinal degradation, the condition often worsens significantly over an 18-month period, shifting from moderate irritation to severe, incapacitating pain. The pain typically originates in the lower back and radiates forcefully downward into the lower extremities, a phenomenon known as radiculopathy. This radiating neuropathic pain drastically restricts walking tolerance and standing endurance, forcing patients to adopt a hunched posture to relieve nerve compression.
Identifying Key Symptoms of Lumbar Nerve Compression
Recognizing the physiological signs of nerve root entrapment is crucial for timely orthopedic intervention. The structural changes, including thickened ligaments and bone spur formation, create distinct neurological deficits. Patients must accurately document their symptom progression to provide spine surgeons with comprehensive diagnostic data.
- Neurogenic Claudication: Severe cramping and pain in the legs that worsens with prolonged standing or walking, but improves when sitting or leaning forward.
- Sciatic Radiating Pain: Sharp, electrical sensations traveling from the lower lumbar segments through the buttocks and down the posterior aspect of the legs.
- Motor Weakness and Sensory Loss: Progressive numbness, tingling sensations, and potential foot drop indicating compromised motor nerve function.
Clinical Assessment and Surgical Consultation Protocols for Spinal Issues
A rigorous pre-operative consultation is the foundation of any successful complex spine procedure. During the initial diagnostic phase around [00:18], spine surgeons evaluate advanced imaging modalities such as high-resolution MRI and CT myelograms. These diagnostic tools allow the surgical team to map the exact locations of stenosis and assess the structural integrity of the intervertebral discs.
Following the radiographic analysis, the consultation pivots to a detailed discussion of therapeutic pathways. Orthopedic specialists present patients with a comparative analysis of traditional manual decompression versus advanced robotic-assisted stabilization. The objective is to formulate a customized surgical blueprint that addresses both the immediate nerve impingement and the long-term biomechanical stability of the vertebral column.
Evaluating Patient Candidacy for Minimally Invasive Approaches
Not all patients with spinal stenosis require extensive reconstructive surgery. Surgeons meticulously assess patient candidacy based on bone density, specific anatomical variations, and the presence of co-morbidities. The goal is to determine the least invasive surgical corridor that will yield maximum neurological decompression.
Factors influencing the surgical strategy include the severity of facet joint hypertrophy and the presence of degenerative spondylolisthesis. If spinal instability is detected alongside stenosis, surgeons will mandate a concurrent fusion procedure to prevent future vertebral slippage. This comprehensive evaluation ensures that the chosen surgical modality aligns perfectly with the patient's unique physiological requirements.
Technological Superiority of Robotic-Assisted Spine Surgery
The integration of robotics into orthopedic surgery represents a monumental leap in procedural safety and biomechanical accuracy. As highlighted during the technical explanation near [00:29], robotic systems act as highly advanced navigational assistants for the primary surgeon. These computerized platforms utilize pre-operative CT scans to generate a three-dimensional, interactive model of the patient's exact spinal anatomy.
During the actual procedure, the robotic arm provides a rigid, unyielding trajectory for the placement of surgical instruments and spinal hardware. This automated guidance system helps guide surgical instruments with sub-millimeter accuracy, drastically reducing the margin of human error. Consequently, the risk of misplacing pedicle screws or causing iatrogenic nerve injury is statistically minimized, directly improving clinical outcomes.
Comparative Analysis: Traditional Versus Robotic Spine Implantation
Understanding the functional differences between manual freehand techniques and robotic navigation is essential for prospective patients. Traditional methods rely heavily on the surgeon's tactile feedback and repeated intraoperative fluoroscopy (X-rays). Conversely, robotics offer real-time tracking and pre-planned virtual trajectories.
| Surgical Factor | Traditional Manual Surgery | Robotic-Assisted Surgery |
|---|---|---|
| Hardware Accuracy | Relies on surgeon experience and direct visual anatomical landmarks. | Provides pre-planned, computerized trajectory guidance with sub-millimeter precision. |
| Radiation Exposure | Requires continuous intraoperative X-rays for instrument verification. | Significantly reduces fluoroscopy dependency, lowering radiation for patient and staff. |
| Tissue Retraction | Often requires larger incisions and more extensive muscle dissection. | Facilitates minimally invasive approaches, reducing surrounding soft tissue trauma. |
Accelerated Post-Operative Recovery and Mobilization Protocols
One of the most profound benefits of utilizing robotic precision in spine surgery is the dramatically reduced post-operative recovery timeline. By minimizing collateral damage to the paraspinal muscles during surgical access, patients experience significantly less inflammatory response and localized pain. Evidence of this rapid mobilization is seen around [00:40], where patients returning to their hospital rooms post-surgery can initiate movement protocols remarkably fast.
Early ambulation is a cornerstone of modern orthopedic recovery. It is entirely common for inpatient physical therapists to assist patients out of bed and walking the morning immediately following a robotic spinal decompression. This proactive approach to physical therapy prevents deep vein thrombosis, stimulates circulation, and accelerates the overall healing trajectory faster than traditional anticipated timelines.
Phases of Post-Surgical Spine Rehabilitation
Rehabilitation following a major spinal intervention requires strict adherence to biomechanical guidelines. Patients must navigate their daily activities while protecting the healing surgical site and allowing bone grafts to fuse successfully. The recovery protocol is divided into distinct, structured phases.
- Acute Inpatient Phase (Days 1-3): Focus on basic mobilization, transferring in and out of bed utilizing the log-roll technique, and managing acute incisional pain.
- Sub-Acute Ambulatory Phase (Weeks 1-4): Gradual increase in daily walking distances. Strict avoidance of bending, lifting, and twisting (BLT protocols) to protect spinal instrumentation.
- Core Stabilization Phase (Months 1-3): Introduction of isometric core strengthening exercises under the supervision of a specialized spine physical therapist to build muscular support.
Strategic Advantages of Medical Tourism for Orthopedic Procedures in Turkiye
The global landscape of healthcare is shifting, with international destinations offering highly competitive medical solutions. Turkiye has emerged as a premier global hub for complex orthopedic procedures, including robotic spinal stenosis surgery. For patients facing prohibitive out-of-pocket costs or extended waitlists in their home countries, traveling abroad presents a highly viable, high-quality alternative.
As noted in patient testimonials around [01:02], thoroughly researching specialized facilities in Turkey reveals a healthcare infrastructure that rivals or exceeds Western standards. International patients benefit from access to globally trained surgical teams, state-of-the-art robotic technology suites, and dedicated international patient coordination departments that handle all logistical friction.
Economic Efficiency Without Compromising Clinical Quality
The economic disparity between US healthcare pricing and international medical centers is a primary driver for medical tourism. The comprehensive cost of robotic spine surgery in Turkey, including hospital stays, surgical fees, and advanced imaging, is often a fraction of domestic estimates. This pricing structure is achieved through lower administrative overhead and advantageous currency exchange rates, not through a reduction in medical supplies or clinical standards.
Furthermore, package pricing offered by international clinics provides financial transparency that is rarely found in traditional healthcare systems. Patients receive upfront, all-inclusive cost estimates that cover the entire continuum of care. This predictable financial model allows patients to invest in superior robotic technology that might have been economically inaccessible in their home nation.
Criteria for Selecting High-Authority International Orthopedic Clinics
Identifying a secure and reputable medical facility abroad requires diligent pre-travel investigation. Prospective patients must look beyond marketing materials and evaluate objective markers of institutional excellence. The most critical factor is verifying international healthcare accreditations, such as Joint Commission International (JCI), which mandates strict compliance with global patient safety and quality control standards.
Equally important is assessing the professional pedigree of the leading orthopedic surgeons. Patients should prioritize clinics directed by specialists who hold leadership positions in recognized medical associations, such as the Robotic Orthopedic Surgery Association. Active involvement in academic research and a high volume of successfully completed robotic spine cases are strong indicators of elite surgical proficiency.
Evaluating Institutional Infrastructure and Patient Support Systems
A top-tier international clinic will possess comprehensive internal infrastructure designed to support complex orthopedic recoveries. This includes dedicated neuro-monitoring units, advanced intensive care facilities, and integrated physical therapy departments located within the same hospital complex. The proximity of these services ensures rapid response to any post-operative clinical needs.
Additionally, the quality of the international patient department is a vital metric for selecting a facility. High-authority clinics provide dedicated case managers who facilitate seamless communication. These professionals handle the translation of medical records, coordinate pre-operative virtual consultations, and manage on-the-ground logistics from airport transfers to accommodation near the medical center.
Comprehensive Risk Management in Complex Spine Interventions
While robotic assistance dramatically lowers intraoperative risks, spinal decompression and fusion remain major surgical undertakings. Understanding the clinical mechanisms employed to mitigate complications is essential for patient peace of mind. Infection control is paramount; leading surgical centers utilize ultra-clean ventilation systems in operating theaters and administer prophylactic antibiotics based on strict international guidelines.
Neurological safety is continuously monitored during the procedure utilizing Intraoperative Neuromonitoring (IONM). This advanced technique tracks the electrical activity of the spinal cord and peripheral nerves in real-time. By providing instantaneous feedback to the surgical team, IONM acts as a critical fail-safe, ensuring that surgical maneuvers do not compromise delicate neural pathways during the decompression process.
Managing Post-Operative Biomechanical Stability
Long-term success following spinal stenosis surgery depends heavily on achieving solid bone fusion, when instrumentation is utilized. Surgeons employ advanced bone grafting materials and precise hardware placement to create an optimal biological environment for osteogenesis. Patients are carefully monitored through follow-up imaging to verify that the vertebral segments are fusing correctly.
To prevent adjacent segment disease—a condition where adjacent spinal levels degenerate due to altered biomechanics—surgeons emphasize precise anatomical alignment during the robotic procedure. Correcting the sagittal balance of the spine ensures that weight-bearing forces are distributed evenly, protecting the remaining healthy discs from excessive mechanical stress over the subsequent years.
Logistical Preparation for Cross-Border Healthcare Journeys
Preparing for international medical travel requires meticulous organizational planning to ensure a stress-free clinical experience. The process begins with securely transferring all pertinent medical records, including high-resolution DICOM files of recent MRI scans, to the chosen international medical team. This allows the orthopedic surgeons to finalize the surgical plan and confirm patient candidacy before travel arrangements are finalized.
Patients must also coordinate travel logistics that accommodate post-operative mobility restrictions. This includes arranging specific seating accommodations for flights and ensuring that the selected hotel in the destination country offers accessible facilities. Effective preparation mitigates travel-related anxiety, allowing the patient to focus entirely on their impending surgical procedure and subsequent physical rehabilitation.
Essential Pre-Travel Medical Clearances
Prior to departure, international patients must undergo comprehensive pre-operative medical clearances in their home country. This typically involves extensive blood panels, electrocardiograms (EKG), and consultations with primary care physicians or cardiologists. Ensuring systemic health stability is mandatory before administering general anesthesia in a foreign medical facility.
- Medication Management Review: Strict instructions must be followed regarding the cessation of blood-thinning medications and certain supplements weeks prior to surgery to prevent intraoperative hemorrhage.
- Travel Visa and Insurance Coordination: Securing appropriate medical visas and verifying if existing health insurance policies offer any out-of-network reimbursement for international emergency care.
- Post-Discharge Support Planning: Arranging for a travel companion or a specialized medical escort to assist with mobility, luggage, and personal care during the return journey home.
Ready to Explore Advanced Spine Surgery Options?
Take the first step toward lasting pain relief. Request a personalized consultation to discuss robotic spinal stenosis surgery and receive a comprehensive, transparent medical travel plan tailored to your specific orthopedic needs.
Get Free QuoteView Full Video Transcript: Patient Success Story
[00:00] My back pain, because I've had degenerative spinal stenosis, it started mild and went to moderate, and in the last year and a half it went into severe from my low back and into my legs.
[00:18] We met with the spine surgeon. He, the choice was to have a manual surgery or robotic, and he believed robotic was going to be the best and he gave us the reasons why.
[00:29] During the procedure, the robot can help guide our surgical instruments with greater accuracy and precision, reducing the risk of complications and improving outcomes.
[00:40] I had the surgery on a Friday morning and was back in my room in the afternoon, and the next morning the physical therapist came in and I got up and walked.
[00:53] So it was a lot quicker recovery from the surgery than I anticipated. Oh I, I feel really good. I'm very happy with the outcome so far.
[01:02] If you're considering having spinal surgery, do some research and check out this facility and give it serious thought.
[01:10] Could have had all this done in the US, that was certainly an option for us, but in the end we chose Turkiye and we're very happy that we did that.



.png)






Share this listing