Advanced Stem Cell Therapy for Lumbar Herniated Discs in Colombia
Chronic lower back pain caused by spinal trauma presents significant challenges for long-term physical mobility. Individuals suffering from degraded spinal discs often seek viable alternatives to invasive surgical procedures. Stem cell therapy for lumbar herniated discs in Colombia has established itself as a leading non-surgical medical intervention.
This highly advanced treatment protocol focuses on cellular regeneration and deep tissue repair rather than temporary symptom management. By utilizing powerful biological agents, clinicians can address the root causes of neuropathic pain and structural instability.
Patients who travel for regenerative medicine receive comprehensive care plans designed to restore their quality of life. The integration of modern cellular therapies provides a scientifically backed pathway to recovery. We will examine the specific clinical steps involved in treating severe spinal conditions using these state-of-the-art protocols.
Video Chapters
Stem Cell Therapy for Lumbar Herniated Discs in Colombia
The Case Study of Kevin Girgis
Many patients endure prolonged periods of physical discomfort following severe orthopedic injuries. At [00:00], the clinical documentation introduces Kevin Girgis, a patient dealing with chronic spinal issues. His specific condition required a targeted approach due to the longevity of the underlying damage.
Medical teams thoroughly evaluated his medical history to determine the most effective regenerative protocol. The assessment confirmed that standard physical therapy and localized corticosteroid injections were insufficient for his needs. A specialized cellular therapy plan was developed to address the exact location of the tissue degradation.
The Impact of Early Sports Injuries
Sports-related trauma during adolescence frequently leads to degenerative joint and spine conditions later in life. As explained at [00:05], Kevin suffered a severe accident while playing soccer at the age of fifteen. This high-impact collision directly compromised his lower back, specifically affecting the lumbar region.
The initial trauma caused micro-tears in the spinal disc, which progressively worsened over the course of fifteen years. Early injuries often disrupt the natural biomechanics of the spine, leading to accelerated wear and tear. This long-term mechanical stress ultimately resulted in a painful herniated disc requiring advanced medical intervention.
Targeted Delivery of Biological Agents
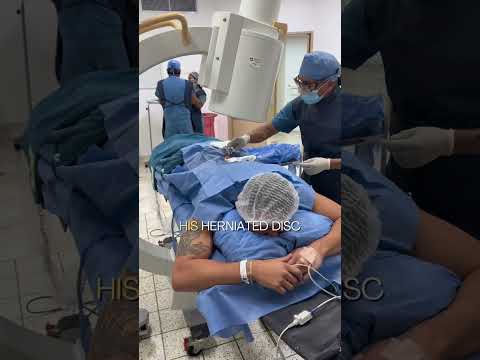
The success of cellular medicine relies heavily on precise administration protocols. At [00:08], the medical staff is shown in the surgical room executing the primary phase of the treatment. The attending physician administered the stem cells directly into the compromised herniated disc.
They also targeted the surrounding facet joints to stabilize the entire lumbar segment. Using advanced fluoroscopic imaging ensures that the biological materials reach the precise areas of tissue damage. This localized application maximizes the therapeutic concentration, encouraging optimal cellular integration and repair.
Understanding the Impact of Lumbar Herniated Discs on Daily Life
The Mechanics of Disc Herniation
The human spine relies on intervertebral discs to absorb shock and facilitate fluid movement. A lumbar herniated disc occurs when the gelatinous inner core breaches the tough outer fibrous ring. This structural failure causes the disc material to protrude outward into the spinal canal.
The localized pressure disrupts the normal anatomical spacing required for nerve roots to exit the spinal column. The mechanical compression immediately triggers intense localized pain and inflammatory responses. Over time, the continuous friction exacerbates the deterioration of the surrounding spinal structures.
Neurological Symptoms and Physical Limitations
Spinal disc protrusions frequently interfere with the central nervous system's communication pathways. Patients routinely experience sharp, radiating neuropathic pain that travels down the buttocks and legs. This condition, commonly known as sciatica, is accompanied by severe numbness and tingling sensations.
The irritation of the sciatic nerve can cause sudden muscle weakness in the lower extremities. These neurological deficits make walking, standing, or sitting for prolonged periods incredibly difficult. Simple daily tasks become monumental physical challenges due to the unpredictable nature of the pain.
The Psychological Toll of Chronic Back Pain
Living with unrelenting physical discomfort significantly impacts an individual's mental and emotional well-being. Chronic back pain severely disrupts natural sleep cycles, leading to profound daytime exhaustion. The inability to participate in social events, sports, or family activities often causes feelings of isolation.
Patients frequently report elevated levels of anxiety and depression linked to their lack of mobility. The ongoing reliance on pharmaceutical pain management further complicates their overall health profile. Addressing the psychological burden requires resolving the underlying physical damage through effective medical therapies.
How Stem Cell Injections for Back Pain Provide Lasting Relief
The Biological Science of Cellular Repair
Regenerative medicine utilizes the body's intrinsic healing mechanisms to repair degraded tissues. Stem cells are undifferentiated biological units capable of developing into highly specialized cells. When introduced into a damaged spinal disc, they actively promote the regeneration of the annulus fibrosus.
These cells release critical growth factors that stimulate localized tissue synthesis and repair. The biological agents work to rebuild the structural integrity of the damaged spinal segment. This process halts the degenerative cascade and initiates a genuine healing response at the cellular level.
Fluoroscopic Guidance for Precision Placement
The administration of cellular therapies requires exact anatomical targeting to achieve desired clinical outcomes. Orthopedic specialists rely on real-time fluoroscopic imaging to guide the injection process safely. This advanced radiographic technique provides continuous internal visualization of the spinal column.
The physician carefully navigates the needle past sensitive nerve roots directly into the affected disc space. Ensuring accurate placement prevents damage to adjacent healthy tissues while maximizing treatment efficacy. This image-guided precision is a fundamental requirement for successful regenerative spinal procedures.
Long-Term Healing and Structural Stability
Unlike pharmaceutical interventions that offer temporary symptom masking, cellular therapies provide enduring structural improvements. The integrated stem cells continue to divide and repair damaged tissues over several consecutive months. This sustained biological activity gradually restores hydration and volume to the desiccated spinal disc.
As the disc regains its natural height and elasticity, the mechanical pressure on surrounding nerves decreases. Patients experience a steady reduction in neuropathic pain alongside improved spinal flexibility. This long-term stabilization frequently eliminates the necessity for future invasive surgical procedures.
The Role of Ozone Therapy in Reducing Spinal Inflammation
The Science of Medical Ozone
Comprehensive regenerative protocols often incorporate complementary treatments to enhance overall cellular efficacy. At [00:18], the clinical video highlights the application of medical ozone therapy as a crucial finalizing step. Medical ozone is a highly reactive, energized form of oxygen consisting of three distinct atoms.
When introduced into the circulatory system, it immediately triggers a cascade of beneficial biochemical reactions. This oxidative conditioning stimulates the immune system and improves oxygen delivery to hypoxic tissues. The enhanced oxygenation is particularly vital for repairing avascular structures like spinal discs.
Neutralizing Free Radicals for Better Healing
Chronic tissue injuries are frequently plagued by elevated levels of oxidative stress. The medical team explains that a primary function of ozone therapy is to eradicate free radicals. Free radicals are unstable molecular byproducts that cause extensive damage to healthy cellular membranes.
Their continuous presence impedes the integration and proliferation of newly injected stem cells. By neutralizing these harmful compounds, ozone creates a highly optimized microenvironment for biological repair. This detoxification process ensures that the regenerative agents can function without biochemical interference.
Shifting to an Anti-Inflammatory State
Prolonged physical trauma typically locks the human body into a perpetual cycle of chronic inflammation. The clinical staff notes that ozone therapy actively changes the inflammatory state of the patient. The treatment effectively downregulates pro-inflammatory cytokines while upregulating protective anti-inflammatory proteins.
This systemic modulation reduces the localized swelling surrounding the compressed spinal nerves. By shifting the physiological baseline to an anti-inflammatory state, the therapy provides immediate symptomatic relief. This biological transition is essential for accelerating the overall timeline of tissue regeneration.
Enhancing Healing with Exosome Therapy for Nerve Regeneration
What Are Extracellular Vesicles?
The latest advancements in biological medicine have isolated the active communicators within cellular treatments. At [00:31], the protocol introduces an additional round utilizing targeted exosome therapy. Exosomes are microscopic extracellular vesicles secreted primarily by mesenchymal stem cells.
They serve as biological delivery vehicles, containing a dense concentration of messenger RNA, proteins, and lipids. These isolated particles do not contain live cellular nuclei, making them incredibly safe and highly bioavailable. Their minuscule size allows them to easily cross biological barriers and penetrate dense fibrotic tissues.
Nano Cell Communicators in Action
The mechanism of action for extracellular vesicles revolves entirely around precise intercellular signaling. The attending physician explicitly describes these elements as tiny nano cell communicators. Once introduced into the spinal canal, they immediately seek out damaged and inflamed local cells.
The exosomes bind to the target cell membranes and transfer their specialized regenerative payload. This exchange of vital genetic information effectively reprograms the damaged cells to begin rapid self-repair. They are particularly effective at initiating remyelination, which is the repair of the protective sheath surrounding damaged spinal nerves.
Synergistic Effects with Stem Cells
Administering isolated vesicles alongside whole-cell therapies creates a highly potent medical synergy. The video confirms that exosomes are utilized to speed up the overall stem cell process. They act as biochemical catalysts, providing the necessary instructional cues for the stem cells to differentiate rapidly.
This combined approach ensures that the primary biological agents work significantly better within the damaged environment. The dual-therapy protocol maximizes tissue synthesis, dramatically reducing patient recovery times. Utilizing this synergistic method represents the absolute forefront of modern regenerative orthopedics.
Traditional Back Surgery vs Regenerative Medicine Alternatives
The Risks of Invasive Spinal Procedures
Conventional medical approaches to severe disc herniation frequently culminate in major orthopedic surgery. Procedures such as microdiscectomies or spinal fusions require significant incisions and the physical cutting of muscles. The surgical removal of disc material permanently alters the structural integrity of the spinal column.
These invasive operations carry substantial risks, including hospital-acquired infections, severe blood loss, and adverse anesthesia reactions. Furthermore, surgical interventions often result in the development of dense scar tissue. This internally generated scar tissue can cause recurrent nerve compression and failed back surgery syndrome.
Preserving Natural Spinal Biomechanics
Regenerative medical therapies prioritize the preservation of the patient's original anatomical structures. By focusing on biological healing, these treatments avoid the mechanical destruction associated with surgical procedures. Cellular injections do not require the removal of bone, ligaments, or vital supportive tissues.
This conservative approach maintains the spine's natural range of motion and weight-bearing capabilities. Preserving the inherent biomechanics prevents the adjacent segment disease often seen following rigid spinal fusions. Patients retain their full physical functionality without the limitations imposed by implanted surgical hardware.
A Comparative Look at Recovery Timelines
The post-procedural experience differs drastically between surgical interventions and biological treatments. Spinal surgery typically demands a prolonged, painful recovery period involving weeks of total bed rest. Patients must undergo months of intensive physical rehabilitation to regain basic mobility and core strength.
Conversely, minimally invasive cellular therapies are performed entirely in an outpatient clinical setting. Patients typically walk out of the facility on the same day and resume light daily activities within a week. This accelerated recovery timeline minimizes disruption to professional careers and personal responsibilities.
- Procedural Approach: Surgical interventions require mechanical tissue alteration, whereas regenerative medicine utilizes needle-based biological delivery.
- Hospitalization Requirements: Conventional operations mandate extended hospital stays; cellular therapies offer rapid outpatient convenience.
- Risk Profile: Open spine surgery carries high risks of infection and scarring; biologic injections maintain an extremely low complication rate.
- Therapeutic Objective: Surgery aims to physically remove pressure; stem cell protocols aim to organically rebuild and heal damaged tissues.
Why Choose Stem Cell Treatment for Herniated Discs in Latin America
Advanced Regulatory Environments for Cellular Medicine
International medical destinations have developed progressive regulatory frameworks supporting advanced biological therapies. Latin American health ministries often approve the clinical use of culturally expanded mesenchymal stem cells. This specific biological cultivation allows physicians to administer exponentially higher cell counts per treatment.
Domestic regulations in North America heavily restrict the manipulation and expansion of harvested cellular tissues. By traveling internationally, patients gain access to robust, highly concentrated therapies that yield superior regenerative outcomes. This regulatory freedom positions the region as a primary hub for specialized orthopedic care.
State-of-the-Art Facilities and Global Expertise
The clinical infrastructure supporting medical tourism in this sector rivals the best hospitals globally. Specialized regenerative clinics feature modern surgical suites equipped with the latest imaging and processing technology. The medical professionals leading these institutions are internationally recognized experts in the field of orthopedics.
Many of the attending physicians have completed advanced fellowships across Europe and the United States. Their deep clinical expertise ensures that every protocol adheres to strict international safety and quality standards. Patients receive world-class medical attention tailored entirely to complex orthopedic conditions.
Comprehensive and Personalized Treatment Protocols
International healthcare facilities excel at providing highly personalized, patient-centric medical experiences. Standard domestic healthcare often limits patient-doctor interaction due to high volume administrative constraints. Conversely, medical tourism clinics design comprehensive, multi-day itineraries focused solely on the individual's recovery.
The integration of auxiliary treatments like intravenous nutrition, ozone, and extracellular vesicles is standard practice. This holistic, all-encompassing approach ensures that every biological variable is optimized for maximum healing. The dedicated attention significantly enhances the overall patient experience and subsequent clinical success.
Exploring the Cost of Stem Cell Therapy for Spinal Issues
Navigating Insurance Limitations in North America
Financing advanced medical treatments presents a significant hurdle for many individuals suffering from chronic pain. Major medical insurance providers routinely categorize biological and cellular therapies as experimental or investigational. Consequently, claims for these highly effective orthopedic treatments are almost universally denied by corporate insurance carriers.
Patients are forced to cover the exorbitant out-of-pocket costs demanded by domestic specialized clinics. These inflated regional prices place transformative regenerative medicine entirely out of reach for the average working individual. This systemic financial barrier prevents thousands from accessing necessary biological healing.
The Economics of Medical Tourism
Traveling internationally for specialized healthcare completely alters the financial landscape of medical treatments. The economic structure of healthcare in Latin America allows for drastically reduced overhead and administrative costs. Clinics pass these substantial operational savings directly onto the patient without compromising clinical quality.
A comprehensive biological protocol abroad often costs a fraction of a single basic injection in domestic markets. Favorable currency exchange rates further maximize the purchasing power of international patients. This economic accessibility democratizes advanced medicine, allowing a broader population to seek effective healing.
Long-Term Financial and Health ROI
Evaluating the true cost of medical care requires analyzing the long-term financial implications of chronic illness. Opting for cellular therapy helps patients avoid the astronomical expenses associated with open back surgery. It eliminates the need for ongoing prescription pain medications, continuous physical therapy, and costly specialized medical equipment.
The rapid recovery timeline allows individuals to return to their professional careers quickly, minimizing lost wages. Ultimately, investing in regenerative medicine yields an immeasurable return regarding physical independence, mobility, and overall life satisfaction. By choosing a biological treatment plan, individuals invest directly in their long-term health and vitality.
Ready to Heal Your Back Pain Without Surgery?
Discover if you are a candidate for advanced stem cell therapy and exosome treatments. Connect with leading orthopedic specialists in Latin America to receive your personalized, free treatment evaluation today.
Get Free QuoteView Full Video Transcript
00:00 Hey guys this is Kevin Girgis and its a patient that had an accident when he was fifteen years old playing soccer his lower back lumbar was affected.
00:08 Yesterday we were at surgical room where we were able to give Kevin the stem cells directly applied to his herniated disc and the facets as well.
00:18 Today is his last day we're doing a round of ozone to finalize the treatment what that helps to do is get rid of free radicals speed up healing and change the inflammatory state of the patient to an anti inflammatory state.
00:31 Aside of that we're gonna do another round of exosomes which are tiny nano cell communicators that are gonna speed up the stem cell process and make sure they work better.















Share this listing