Transformative Hip Replacement Surgery in Mexico for Lasting Mobility
Living with chronic joint pain can severely diminish your quality of life, making a highly specialized and advanced hip replacement surgery in Mexico a profound step toward reclaiming your independence. When conservative treatments no longer provide relief for severe joint degradation, exploring international orthopedic options can connect patients with world-class medical expertise. Addressing progressive arthritis through a precise surgical intervention not only alleviates debilitating discomfort but also completely restores fundamental biomechanical function.
Understanding the patient journey provides invaluable clinical insight into what you can expect from complex orthopedic care. For instance, individuals like Aaron, a 70-year-old patient, have shared extensive details about their transformative joint replacement experiences [00:06]. By examining real-world medical cases, prospective patients can better comprehend the long-term implications of untreated skeletal trauma and the remarkable efficacy of modern joint prosthetics.
Video Chapters
- The Biomechanics of Post-Traumatic Joint Degradation
- Identifying the Domino Effect of Compensatory Walking
- Comprehensive Diagnostic Protocols for Advanced Wear
- Formulating a Strategic Orthopedic Treatment Plan
- Detailed Breakdown of the Total Hip Prosthesis Procedure
- Exploring the Benefits of Orthopedic Medical Tourism
- Structured Hip Replacement Rehabilitation Timeline
- Long-Term Maintenance and Low-Impact Sports
The Biomechanics of Post-Traumatic Joint Degradation
Traumatic injuries often serve as the hidden catalyst for severe orthopedic complications that surface decades later. An initial accident can fundamentally alter the structural integrity of the skeletal system, leading to long-term vulnerabilities. Many patients trace their severe joint issues back to a specific traumatic event, such as a major fall or high-impact collision [00:15].
These initial impacts can cause complex, fragmented fractures, including severe breaks in the hip and ankle regions. Managing an exposed fracture requires immediate, intensive surgical care to stabilize the bones and prevent catastrophic infection [00:26]. Even with successful primary surgeries, the original physical trauma permanently disrupts the smooth articular cartilage covering the bone ends.
Anatomy of a Compromised Hip Joint
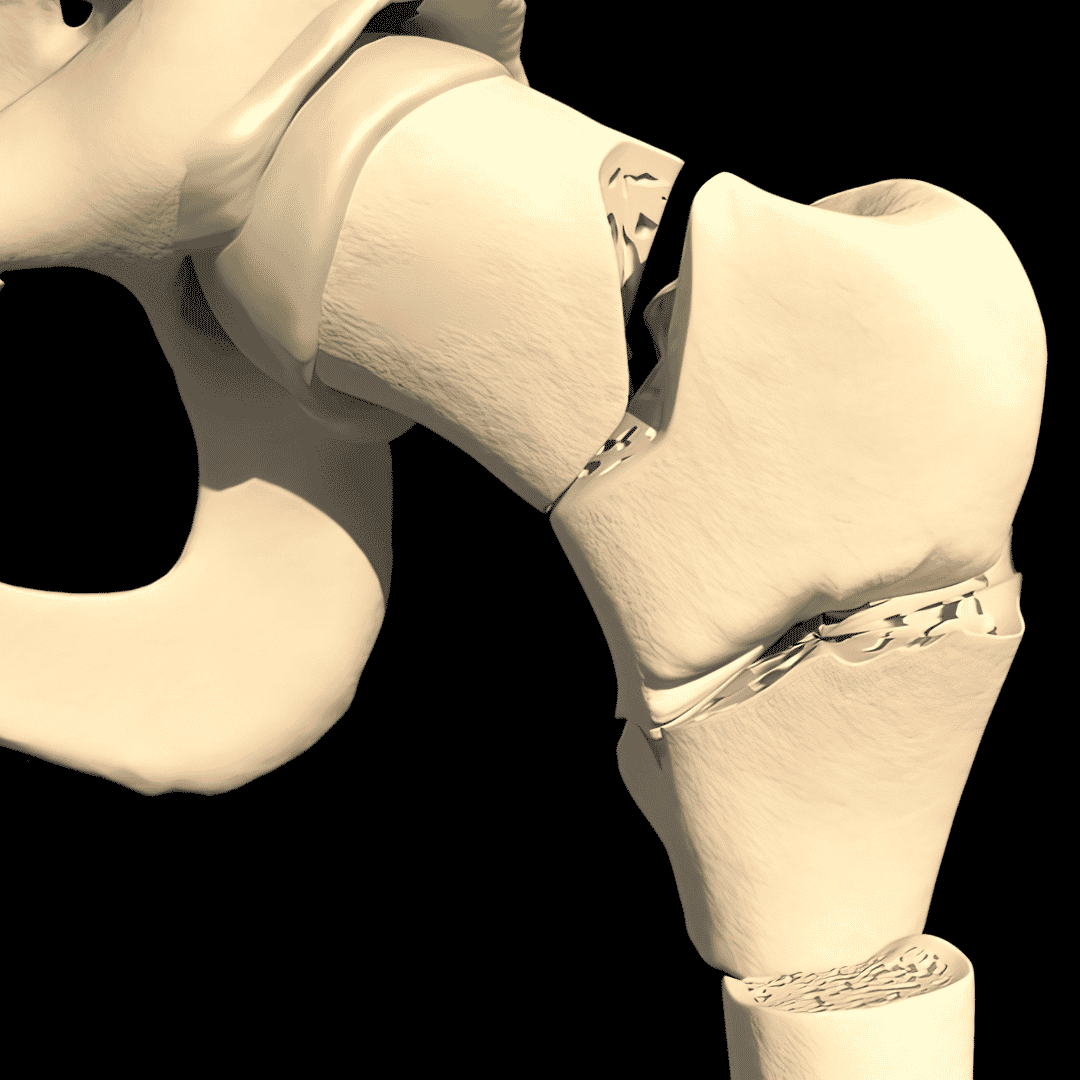
To fully comprehend the necessity of orthopedic intervention, one must understand the intricate mechanics of a healthy human hip joint. It operates as a classic ball-and-socket mechanism, where the spherical femoral head rests perfectly within the cup-like acetabulum of the pelvis. This vital junction is responsible for supporting the entire weight of the upper body while facilitating a massive range of dynamic, multidirectional movements.
In a perfectly healthy state, both the ball and the socket are coated with a thick, frictionless layer of articular cartilage. This protective tissue is continuously lubricated by synovial fluid, allowing the bones to glide seamlessly against one another. When trauma strips this cartilage away, the resulting bone-on-bone friction triggers severe inflammation and immediate structural degradation.
The Onset of Post-Traumatic Arthritis
Over time, this disrupted cartilage cannot regenerate effectively, leading to a specialized condition clinically known as post-traumatic arthritis. The uneven joint surfaces create abnormal friction during movement, slowly wearing away the remaining protective cushioning over several years. This progressive deterioration explains why individuals experience a relatively normal period of mobility before debilitating symptoms finally emerge.
The cellular breakdown within the joint space accelerates as the micro-traumas accumulate from daily walking and standard weight-bearing activities. Inflammatory enzymes flood the joint capsule, further degrading the synovial fluid's natural lubricating properties. This relentless cycle of friction and internal inflammation eventually destroys the underlying subchondral bone structure.
Identifying the Domino Effect of Compensatory Walking Patterns
When one limb is compromised by injury or subsequent corrective surgeries, the human body naturally attempts to compensate to maintain an upright balance. Often, patients must utilize specialized orthopedic devices, such as custom shoe inserts or heel lifts, to correct resulting leg length discrepancies. Wearing a corrective insole in the affected foot becomes a daily necessity to facilitate a relatively normal, fluid walking pattern [00:43].
While these supportive devices are highly essential for immediate rehabilitation, they can inadvertently shift the body's mechanical load over the long term. The healthy, uninjured leg often takes on a significantly higher percentage of the individual's body weight to unconsciously protect the previously fractured limb. This chronic, uneven weight distribution places extraordinary mechanical stress on the contralateral joint structures.
Accelerated Wear on the Contralateral Femur
Consequently, the femur on the uninjured side may begin to experience accelerated wear and tear due to this continuous daily overload [00:54]. The cartilage in the previously functional hip breaks down at a much faster rate than it would under normal, symmetrical anatomical conditions. This biomechanical domino effect highlights exactly why comprehensive monitoring of the entire skeletal system is necessary following a localized limb injury.
The pelvis tilts abnormally to accommodate the artificial lift, fundamentally altering the angle at which the femoral head sits deep in the acetabulum. This chronic misalignment causes severe edge-loading, where the physical pressure is concentrated on a very small surface area of the cartilage. Such concentrated force rapidly shears away the hyaline cartilage, exposing the highly sensitive nerve endings buried in the bone.
The Progression of Secondary Joint Pain
As compensatory mechanics take their toll, the onset of secondary joint pain is often insidious, beginning merely as a mild ache. Patients typically endure this mounting pain for several years, falsely attributing it to general aging or residual soreness from their original injuries. However, the pain eventually escalates aggressively, severely restricting basic daily activities and demanding dedicated medical attention [01:05].
This secondary joint pain often radiates from the groin area directly down the anterior thigh, a classic clinical symptom of severe hip pathology. Simple daily tasks like tying shoes, climbing household stairs, or getting out of a low chair become excruciatingly difficult and exhausting. The total loss of internal rotation is usually the first noticeable physical restriction as the thick joint capsule tightens and inflames.
Comprehensive Diagnostic Protocols for Advanced Femoral Wear
When the pain advances and begins to severely restrict basic daily activities, seeking a specialized orthopedic medical evaluation becomes immediately imperative. Consulting with an experienced orthopedic specialist, such as Dr. Eleazar Garcia, provides the highly specific expertise required to accurately diagnose the root cause [01:23]. A thorough clinical examination involves assessing the joint's complete range of motion, pinpointing exact areas of tenderness, and visually evaluating the patient's current gait.
These initial physical assessments provide the foundational clues regarding the true extent of the internal joint degradation and structural deformity. The physician will carefully check for limb length discrepancies and measurable muscle atrophy in both the gluteal and quadriceps muscle groups. A positive Trendelenburg sign during observation often indicates profound weakness in the hip abductors, further confirming severe biomechanical joint dysfunction.
Advanced Radiographic Imaging Techniques
To confirm the clinical diagnosis definitively, physicians rely heavily on advanced diagnostic imaging, primarily utilizing high-resolution X-rays of the pelvis. These specific radiographic images allow the orthopedic surgeon to clearly observe the severe narrowing of the joint space, which definitively indicates massive cartilage loss [01:29]. By directly comparing current X-rays to older baseline images, medical professionals can accurately track the exact progression of the femoral wear.
In addition to standard weight-bearing X-rays, surgeons may frequently order Magnetic Resonance Imaging (MRI) or Computed Tomography (CT) scans for a precise 3D perspective. These advanced imaging modalities reveal hidden soft tissue damage, the presence of subchondral bone cysts, and the exact density of the surrounding pelvic bone. Accurate digital bone mapping is absolutely essential for preoperative surgical planning and selecting the precise geometrical size of the artificial implant.
Identifying Rapidly Progressive Osteoarthritis
In certain complex clinical scenarios, the cartilage destruction is abnormally fast, leading physicians to definitively diagnose rapidly progressive arthritis [01:42]. This highly aggressive form of joint disease quickly strips the joint of its natural protective layers, causing an extremely rapid onset of severe physical disability. The femoral head may even begin to visibly collapse or flatten on the scans, losing its essential spherical shape completely.
Documenting this rapid disease progression is absolutely critical for acquiring insurance authorizations and clinically justifying immediate surgical scheduling. The physician carefully notes the rapid formation of large osteophytes, or jagged bone spurs, which the body creates in a futile biological attempt to stabilize the rapidly deteriorating joint.
Formulating a Strategic Orthopedic Treatment Plan
Once advanced diagnostic imaging confirms the extreme severity of the joint deterioration, the medical team must quickly develop a highly targeted intervention strategy. This aggressive form of bone-on-bone arthritis renders conservative treatments like oral analgesics, localized corticosteroid injections, or extended physical therapy largely ineffective. When the structural bone damage reaches a critical threshold, the raw friction between the bare bones causes excruciating pain and profound mechanical stiffness.
At this advanced pathological stage, the orthopedic surgeon will typically determine that natural joint preservation is no longer a viable or ethical medical option. The definitive clinical recommendation shifts entirely from temporary symptom management to total structural replacement to effectively restore the patient's quality of life. Consequently, the general medical consensus will strongly advise the patient to undergo a comprehensive total hip prosthesis procedure [01:52].
The Decision to Proceed with Arthroplasty
Making the final decision to undergo major orthopedic joint surgery involves careful clinical consideration of the patient's overall health and functional lifestyle goals. The strategic treatment plan is precisely designed to entirely remove the diseased biological components and securely introduce highly durable, artificial mechanics. Preparing the patient mentally and physically for this highly significant surgical intervention is the next crucial phase of the complex orthopedic journey.
Medical optimization prior to surgery strictly includes managing underlying chronic conditions like hypertension or diabetes to ensure a perfectly safe operative environment. The dedicated surgical team conducts comprehensive lab bloodwork and resting electrocardiograms to verify the patient can safely tolerate prolonged general or spinal anesthesia.
Comparison of Joint Treatment Modalities
| Treatment Type | Mechanism of Action | Long-Term Efficacy for Severe Arthritis |
|---|---|---|
| Corticosteroid Injections | Reduces localized joint inflammation temporarily. | Low. Provides short-term pain relief but does not repair structural cartilage damage. |
| Intensive Physical Therapy | Strengthens surrounding musculature to support the joint. | Moderate. Improves mobility but cannot reverse bone-on-bone friction in advanced stages. |
| Total Joint Arthroplasty | Surgical replacement of diseased bone with synthetic implants. | High. Offers definitive correction, eliminating arthritic pain and restoring normal kinematics. |
Detailed Breakdown of the Total Hip Prosthesis Procedure
Undergoing a total hip replacement surgery is a major medical milestone that involves meticulous surgical precision and advanced biomedical engineering. The operation is specifically designed to completely eradicate the primary source of the arthritic pain by excising the severely damaged femoral head entirely. Patients who confidently proceed with the operation often find the structural mechanical correction to be immediately and profoundly transformative [02:01].
During the complex procedure, the orthopedic surgeon implants a highly durable artificial joint, navigating complex anatomical structures with extreme clinical care. The prosthetic titanium stem is securely anchored within the hollow medullary canal of the femur, creating a solid, unmoving foundation for the new joint. A specialized titanium shell cup is then precisely press-fit into the surgically reshaped pelvic bone to serve as the new artificial acetabulum.
Advanced Implant Materials and Design
Modern orthopedic joint implants are meticulously constructed from a sophisticated combination of medical-grade titanium, highly porous metals, and advanced aerospace ceramics. A perfectly smooth, synthetic liner made of highly cross-linked polyethylene is placed safely between the metal components to accurately replicate healthy human cartilage. This extremely low-friction environment guarantees the joint moves naturally and heavily minimizes microscopic wear debris over decades of continuous use.
- Highly Cross-Linked Polyethylene: A dense plastic used for the acetabular liner that dramatically reduces the rate of microscopic wear.
- Porous Titanium Alloys: Used for the femoral stem to encourage natural bone ingrowth and long-term structural fixation.
- Biolox Delta Ceramics: Utilized for the femoral head due to their extreme hardness, scratch resistance, and low friction coefficient.
Minimally Invasive Surgical Techniques
Advancements in modern surgical methodology, such as the highly popular direct anterior approach, allow surgeons to navigate entirely between major muscle groups. Rather than detaching or cutting through vital hip tendons, the surgeon skillfully utilizes natural intermuscular planes to access the thick hip capsule. This tissue-sparing technique significantly reduces intraoperative blood loss, dramatically decreases immediate postoperative pain, and heavily accelerates the initial healing timeline.
Intraoperative fluoroscopic imaging is frequently used during the operation to visually confirm the perfect alignment and absolute leg length equality in real-time. The highly precise spatial orientation of the new prosthetic components is absolutely critical to ensuring long-term mechanical stability and definitively preventing premature implant failure.
Exploring the Benefits of Orthopedic Medical Tourism
When facing a complex medical need, exploring an advanced orthopedic procedure abroad provides an incredible combination of deep affordability and elite surgical expertise. The close geographical proximity of specialized international clinics makes it an easily accessible option for North American patients seeking immediate, high-quality joint relief. Top-tier medical facilities in these specialized health corridors are fully equipped with state-of-the-art robotic surgical assistants and the latest advanced sterilization technologies.
Patients seeking a total hip prosthesis procedure benefit immensely from comprehensive care packages that effectively streamline the entire complex medical journey. These all-inclusive packages often seamlessly bundle the private hospital stay, intricate surgical fees, premium prosthetic hardware costs, and daily dedicated physical therapy sessions. This highly transparent pricing model completely eliminates the financial unpredictability often associated with complex orthopedic surgeries in standard domestic healthcare systems.
Access to World-Renowned Orthopedic Surgeons
The attending physicians and lead surgeons operating in these specialized international hospitals are frequently board-certified by highly respected global medical organizations. These specialized experts perform hundreds of successful joint replacements annually, refining their surgical techniques to an exceptionally high, world-class standard. They strictly utilize the exact same FDA-approved implant materials and high-end surgical instrumentation found in premium, top-ranked hospitals across the United States.
This completely uncompromised standard of clinical excellence strictly ensures that international patients receive highly durable, high-performance joint replacements that are meticulously designed to last. The fully bilingual medical staff provides continuous, crystal-clear communication from the very first diagnostic consultation entirely through the final postoperative medical discharge.
Navigating the International Healthcare Journey
Coordinating complex medical care across borders is seamlessly managed by specialized health facilitators who act as direct liaisons between the patient and the hospital. These dedicated professionals handle all the complex logistical details, including gathering preoperative medical records, scheduling priority surgical dates, and arranging comfortable local hotel accommodations. This dedicated logistical support completely removes the high stress of medical planning, allowing the patient to focus entirely on their upcoming physical recovery.
The standard of rigorous postoperative care in top international clinics often includes extensive daily visits from the lead orthopedic surgeon, a rarity in many domestic systems. This highly personalized attention guarantees that any potential medical complications are quickly identified and addressed immediately during the critical, acute healing phase.
Structured Hip Replacement Rehabilitation Timeline
The total mechanical success of a joint replacement is not solely dependent on the surgical execution; rigorous, daily postoperative rehabilitation is equally vital. Advanced surgical techniques and modern multimodal pain management protocols allow highly motivated patients to begin their physical recovery almost immediately upon waking. Remarkably, many individuals are heavily encouraged to stand and begin walking with therapeutic assistance within three to four short days of the operation [02:08].
This incredibly rapid and deliberate joint mobilization is entirely essential for completely preventing dangerous postoperative complications, such as deep vein thrombosis or fatal pulmonary embolisms. It also strictly prevents the formation of dense, fibrous scar tissue that can permanently restrict the joint's final, desired range of motion. Early weight-bearing safely stimulates the natural bone-growth process necessary to firmly lock the porous titanium implant into the surrounding living skeletal structure.
Targeted Physical Therapy Protocols
Professional orthopedic physical therapists strictly guide recovering patients through highly specific, targeted rehabilitation exercises designed to quickly rebuild the atrophied hip musculature. Total dedication to these progressive, daily exercise routines is the absolute primary driver for restoring full muscular strength and ultimate joint flexibility [02:14]. The initial bed exercises focus entirely on basic isometric muscle contractions, such as heavy gluteal squeezes and rapid ankle pumps, performed while resting in bed.
The physical rehabilitation phase carefully progresses from safely utilizing heavy walking aids like standard walkers to eventually achieving fully independent, unassisted strides. Patients meticulously learn new ways to perform basic daily tasks safely, adhering strictly to temporary movement precautions to totally prevent painful prosthetic dislocation. Through consistent, dedicated therapeutic effort and clear clinical guidance, the strict timeline for returning to a highly functional state is remarkably predictable.
Key Phases of Arthroplasty Recovery
- Days 1-4 (Acute Phase): Focus on immediate joint mobilization, heavy pain management, and smoothly transitioning from a walker to a cane while navigating flat hospital surfaces.
- Weeks 2-6 (Intermediate Phase): Outpatient physical therapy officially begins. Patients work diligently on restoring normal gait mechanics, climbing household stairs safely, and regaining normal driving privileges.
- Months 3-6 (Advanced Phase): Returning confidently to work, engaging in specific low-impact recreational activities, and continuing muscular strengthening to heavily support the new joint architecture.
Long-Term Maintenance and Returning to Low-Impact Sports
The ultimate clinical goal of complete joint arthroplasty is to flawlessly return the individual to a vibrant, highly active lifestyle completely free from the tight constraints of chronic pain. As the dense surrounding muscles finally strengthen and the natural bone fully integrates with the implant, patients experience a profound, lasting restoration of normalcy. They are once again totally able to engage completely in their regular daily routines, walking very comfortably and confidently without a second, painful thought [02:21].
This joyous return to completely independent mobility drastically improves the patient's overall cardiovascular health and significantly boosts their general psychological well-being. Normal activities that were previously considered absolutely impossible, such as grocery shopping or taking long evening walks, become enjoyable aspects of daily life once again. The incredibly heavy burden of chronic arthritic pain is fully lifted, allowing individuals to focus entirely on their physical fitness and long-lost personal hobbies.
Engaging in Joint-Friendly Physical Activities
To safely maintain the long-term health of the cardiovascular system and the extended longevity of the implant, orthopedic specialists highly recommend engaging in low-impact physical activities. Swimming is widely considered particularly beneficial, as the natural physical buoyancy of the water provides excellent, safe resistance training without placing heavy concussive stress on the new joint [02:29]. Using a standard stationary bicycle is another highly excellent method for building dense quadriceps strength while maintaining perfect, safe pelvic stability.
Intelligently integrating these highly safe forms of exercise into a consistent weekly routine ensures that the supporting hip musculature remains robust and highly resilient. A strong, thick muscular envelope effectively acts as a primary physiological shock absorber, physically protecting the synthetic metal components from excessive mechanical wear over vast amounts of time.
Living a Normal Life with a Prosthesis
Ultimately, the complete biological transformation from severely debilitating progressive arthritis to completely unrestricted, fluid movement is a total triumph of modern medical science. The highly successful surgery easily allows patients to live a perfectly normal life, completely indistinguishable in basic mobility from those without complex artificial prosthetics [02:36]. This incredible, pain-free outcome strongly underscores the truly life-changing value of expertly performed orthopedic joint surgery and dedicated, patient-driven postoperative care.
By heavily researching and choosing the absolute right medical surgical team and committing fully to the rigorous, sometimes painful recovery process, individuals can firmly secure decades of highly active, pain-free living. Routine follow-up digital X-rays taken every few years simply ensure the titanium implant remains securely fixed in the bone and performing optimally for the exceptionally long term.
Ready to Reclaim Your Mobility?
Don't let chronic joint pain permanently limit your daily life any longer. Connect directly with world-class orthopedic specialists and confidently explore affordable, highly advanced joint replacement options specifically tailored to your precise medical needs.
Get Free QuoteView Full Video Transcript
00:00
Health Facilitators Phone +1 713-360-4638 info@healthfacilitators.com www.healthfacilitators.com
00:05
Aaron, 70 years, Hip Prosthesis. Hola, buenas tardes, mi nombre es Aaron y quiero hacer participe a la gente que me ve y me escucha.
00:12
I want to give a testimony, on an accident I had in the year 1996. De un testimonio sobre un accidente que tuve en el año del 96.
00:20
In that date I had an accident, had hip fracture and exposed ankle as a result had to have surgery, with a process of rehabilitation of one year.
00:42
I put a staff in his right foot to walk, in the following years to develop my life normally.
00:54
But as a result using the template wear was generated in the left femur.
01:05
I started to have discomfort as consequences of wear femur of his left foot, the inconvenience presented for several years, starting with a pain that was advancing and increasingly hard to get with Dr. Eleazar Garcia.
01:25
Who began to give me treatment and care, to take x-rays to observe the progress in wear femur of his left foot.
01:38
After treatment I indicated that the wear was progressive and accelerated by the artiritis I have.
01:48
So it was determined necessary to develop a prosthetic hip, the operation was carried out in 2008 and I think it was very successful.
02:05
With a very fast recovery, started walking at 3 or 4 days, take rehabilitation exercises and I recovered quickly and began to develop my normal life.
02:22
With issues of daily life such as walking well, including exercise such as swimming and other exercises in the club.
02:35
Actually I have a normal life like any other person.
02:43
I appreciate the help of Dr. Garcia and rehabilitation provided me.
02:51 - 03:06
[Visuals of patient walking independently and Health Facilitators contact information displayed on screen]





-Surgery-in-Mexico-for-US-Travelers-(2).png)









Share this listing