Finding effective ankylosing spondylitis treatment in Turkey has become a major priority for international patients seeking world-class rheumatology care. This chronic inflammatory condition primarily targets the spine, leading to severe daily discomfort and restricted joint mobility over time. Expert rheumatologists emphasize the absolute importance of early detection to prevent permanent spinal fusion and irreversible structural damage. Turkey has steadily emerged as a leading global destination for managing complex autoimmune conditions due to its highly advanced medical infrastructure.
Many patients suffer from debilitating back pain for years without ever realizing they have a systemic inflammatory disease. Medical centers in Turkey offer comprehensive diagnostic panels, including advanced MRI imaging and genetic testing, to accurately identify the root cause of the discomfort. Proper medical management of spondyloarthritis not only alleviates immediate pain but also significantly improves long-term functional quality of life. By choosing specialized Turkish clinics, patients gain direct access to multidisciplinary medical teams dedicated to tailored, highly effective therapeutic approaches.
Video Chapters
Recognizing the Early Symptoms of Ankylosing Spondylitis in Adults
Identifying the warning signs of inflammatory spine conditions can save patients years of unnecessary physical discomfort and mobility issues. At [00:31], the rheumatologist points out that patients frequently experience severe lower back pain during the night. This specific timing is a classic hallmark indicator that the back pain is systemic and directly linked to an overactive immune response.
Patients dealing with this condition often wake up feeling extremely stiff, struggling significantly to get out of bed or perform standard morning routines. This intense morning stiffness typically lasts for more than thirty minutes and only begins to subside as the person engages in physical activity. General medical practitioners sometimes miss these highly specific timing patterns during standard consultations, leading to delayed specialist referrals.
Another major diagnostic red flag is the age at which these specific back pain episodes begin to manifest in the patient. The medical diagnostic criteria specifically target individuals who are under forty-five years old when their back issues first systematically appear. Experiencing persistent, deep back discomfort at a relatively young age strongly points toward an underlying autoimmune issue rather than standard physical wear and tear.
The Impact of Morning Stiffness on Daily Life
For a definitive clinical suspicion of the disease, these inflammatory symptoms must persist without interruption for an extended period. Medical professionals look for continuous lower back pain lasting more than three months before officially confirming an autoimmune spine condition. Short-term back pain resulting from muscle strains, heavy lifting, or minor sports injuries usually resolves well within this specific timeframe.
Ignoring these prolonged symptoms can eventually lead to irreversible structural changes in the spinal column and surrounding pelvic joints. Early medical intervention focuses entirely on managing the internal inflammation before it triggers the vertebrae to permanently fuse together. Seeking a specialized rheumatology evaluation promptly ensures a significantly better long-term prognosis and preserves the patient's natural spinal flexibility.
- Persistent Discomfort: Uninterrupted lower back pain that lasts continuously for more than three months without natural resolution.
- Night Wakings: Severe aching that specifically disrupts sleep patterns, especially during the second half of the night.
- Gradual Onset: Inflammatory pain that slowly intensifies over weeks rather than resulting from a sudden physical injury.
How Sacroiliac Joint Inflammation Triggers Spinal Issues
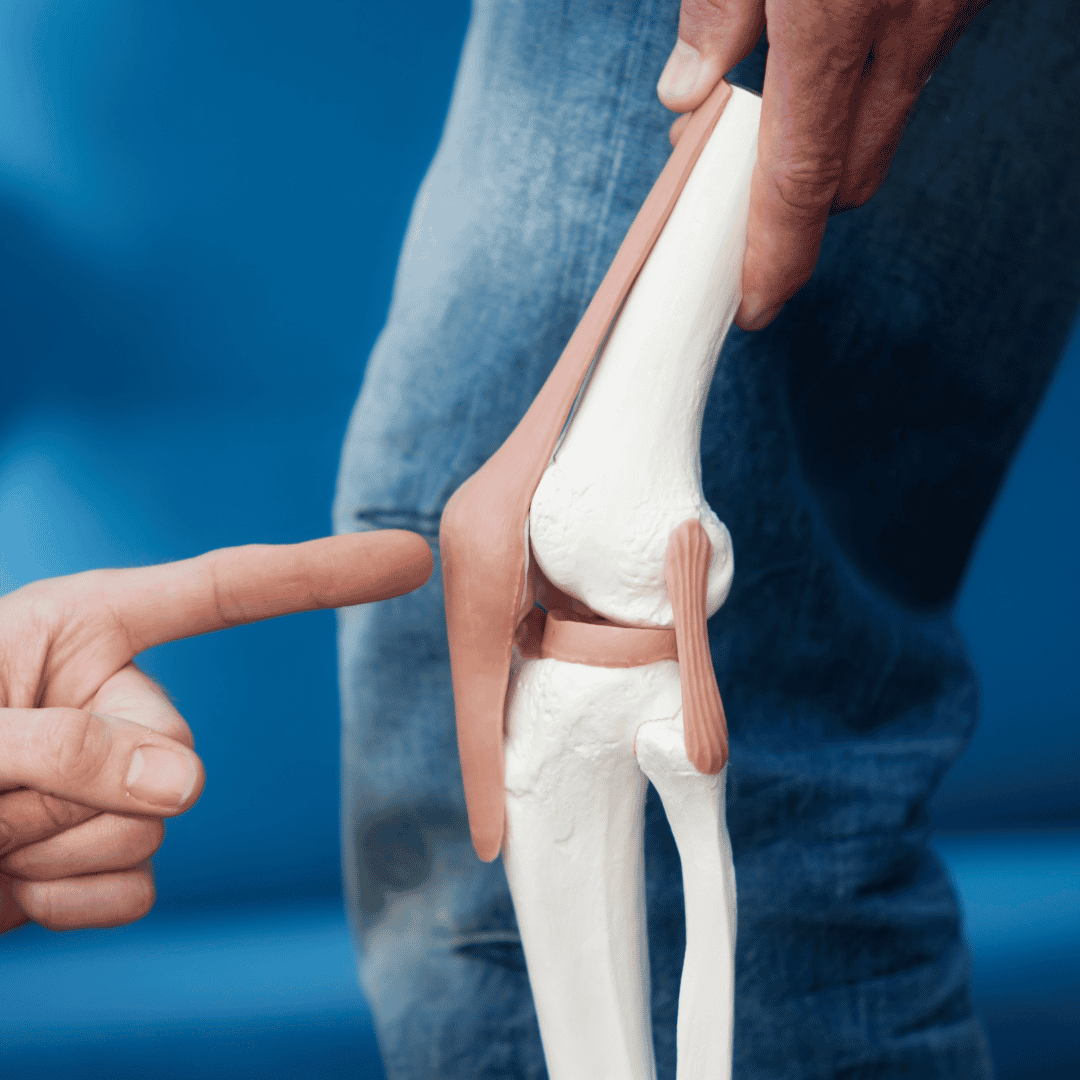
The anatomical origin point of the disease is a critical factor in understanding exactly how the condition spreads through the human body. The specialist explains at [00:05] that the inflammation usually begins in the sacroiliac joint, located deep in the lower back. This specific joint serves as the crucial structural connection between the base of the tailbone and the main pelvic framework.
When chronic inflammation targets the sacroiliac joint, it causes a deep, highly localized aching sensation right around the buttocks and lower lumbar region. Because this specific joint supports the entire structural weight of the upper body, any swelling here makes standing and walking quite painful. Many patients initially confuse this specific joint pain with generic sciatica or a simple pulled muscle in the lower hip area.
As the disease remains medically untreated, the localized pelvic inflammation does not just stay confined to the lower back region. The autoimmune response actively begins to travel upward, systematically attacking the individual vertebrae and ligaments of the spinal column. This continuous upward disease progression is what ultimately leads to the severe physical stiffness associated with advanced stages of the condition.
The Upward Progression of Spine Fusions
Once the active inflammation reaches the higher segments of the spine, the body's natural cellular healing process actually works entirely against it. The immune system attempts to heal the chronically inflamed areas by forming brand new bone tissue between the affected spinal vertebrae. Over a period of several years, this abnormal bone growth fully bridges the gaps between the spinal bones, locking them into a rigid position.
This permanent skeletal fusion dramatically restricts the patient's natural range of motion, making it structurally impossible to bend or twist normally. The newly rigid spine becomes much more susceptible to severe fractures, even from very minor physical impacts or small accidental falls. Preventing this irreversible spinal fusion is the absolute primary goal of modern rheumatology interventions and targeted biologic drug therapies.
Understanding this distinct anatomical progression highlights exactly why catching the disease at the early sacroiliac stage is so medically vital. Halting the immune system's inflammation before it aggressively climbs up the spinal column preserves the patient's mobility and prevents severe postural deformities. Regular medical monitoring through specialized imaging helps doctors track any upward movement and carefully adjust medications accordingly.
Differentiating Between Inflammatory and Mechanical Back Pain
One of the absolute most important clinical distinctions in rheumatology is separating standard mechanical back problems from systemic inflammatory conditions. Mechanical back pain usually stems directly from a specific physical injury, a bulging spinal disc, or general muscle fatigue from heavy lifting. In stark contrast, inflammatory back pain is entirely driven by an overactive immune system mistakenly attacking perfectly healthy joint tissues.
The rheumatologist clearly outlines this vital functional difference at [00:21], noting that patients with inflammatory issues actually feel significantly worse when they rest. If someone with purely mechanical pain lies down on a soft couch, their pain typically subsides rapidly as the physical load is removed. However, a patient with an active autoimmune spine condition will quickly find that physical resting only intensifies their deep lower back discomfort.
This highly counterintuitive physiological reaction to rest is what frequently confuses both affected patients and inexperienced general healthcare providers. When the body remains completely still, the inflammatory chemical markers pool in the affected joints, increasing tissue swelling and causing deep aching sensations. Moving around physically helps circulate the blood and flush out these inflammatory cells, providing reliable, temporary natural pain relief.
| Clinical Feature | Inflammatory Back Pain | Mechanical Back Pain |
|---|---|---|
| Age of Symptom Onset | Usually under 45 years old | Any age, frequently older adults |
| Response to Rest | Actively worsens pain and stiffness | Significantly improves pain levels |
| Response to Movement | Improves daily pain and joint stiffness | Actively worsens physical pain levels |
| Morning Stiffness Duration | Consistently lasts longer than 30 minutes | Brief, usually resolves very quickly |
Why Rest Makes Autoimmune Spine Pain Worse
Because physical inactivity breeds more pain, patients frequently find themselves completely unable to sleep through the night peacefully. The prolonged stillness of a normal sleeping cycle allows the joint inflammation to peak, which is exactly why the pain frequently wakes them up before dawn. This chronic sleep disruption rapidly leads to severe daytime fatigue, compounding the heavy physical exhaustion caused by the active autoimmune disease itself.
Consistent physical activity, gentle daily stretching, and highly specialized exercises are inherently beneficial for individuals suffering from autoimmune joint issues. Engaging in smooth, low-impact movements like swimming or tailored yoga keeps the spine flexible and actively reduces the dangerous pooling of inflammatory cells. Medical professionals heavily incorporate structured movement therapies into the overall clinical management plan for these specific joint conditions.
Failing to clinically recognize the strict difference between these two types of pain often leads to completely ineffective medical treatment strategies. Prescribing strict bed rest for an inflammatory spine condition will actively worsen the patient's immediate symptoms and rapidly accelerate joint stiffness. Accurate early diagnosis relies heavily on taking a very detailed patient history regarding exactly how their daily pain responds to physical activity versus prolonged sitting.
Diagnostic Procedures for Autoimmune Spine Conditions in Turkey
Turkey has firmly established itself as a premier global hub for diagnosing complex autoimmune diseases with incredibly high medical accuracy. The initial diagnostic journey usually begins with a highly thorough clinical interview focusing strictly on the precise timing and physical triggers of the patient's back pain. At [00:51], the specialist details how inflammatory back pain symptoms directly prompt the immediate need for specific radiological imaging.
Standard medical X-rays are typically the absolute first imaging tool utilized to look for clearly visible structural damage in the pelvic region. Expert radiologists specifically examine the sacroiliac joint to reliably identify any distinct signs of bone erosion, tissue sclerosis, or early joint space narrowing. If these distinct structural changes are clearly visible on the standard X-ray, confirming the final clinical diagnosis becomes a relatively straightforward medical process.
However, standard X-ray imaging has highly significant technical limitations when it comes to catching the autoimmune disease in its absolute earliest stages. Visible bone damage often takes multiple years to fully develop, meaning a patient could suffer from severe active inflammation long before an X-ray shows anything definitively abnormal. Relying purely on basic X-rays can inadvertently delay highly necessary medical interventions for patients actively experiencing intense, daily debilitating pain.
The Role of X-Rays and MRI in Rheumatology
To fully overcome the strict technical limitations of standard radiography, top medical centers in Turkey heavily utilize advanced Magnetic Resonance Imaging (MRI). A high-resolution MRI scan can easily detect active bone marrow edema and hidden soft tissue inflammation well before any permanent structural bone damage actually occurs. This crucial level of early medical detection is completely impossible to achieve with traditional, older X-ray technology.
Using modern MRI technology allows highly trained rheumatologists to intervene aggressively while the structural joint disease is still entirely reversible. By explicitly confirming the presence of active cellular inflammation early, doctors can immediately prescribe targeted biologic medications to safely suppress the patient's immune response. This proactive, technology-driven diagnostic approach drastically improves the long-term health outcomes for international patients seeking specialized care in modern Turkish hospitals.
The strategic integration of targeted genetic testing also plays a highly vital supportive role in the comprehensive rheumatology diagnostic workup. Testing specifically for the HLA-B27 genetic marker helps medical doctors build a much stronger clinical case, especially when radiological imaging results are slightly ambiguous. Combining a detailed patient history, advanced MRI scans, and specific genetic profiling ensures a highly accurate, definitive diagnosis for complex spinal conditions.
Understanding Non-Radiographic Axial Spondyloarthritis Diagnosis
Not every autoimmune patient fits perfectly into the classic medical diagnostic mold, which can severely complicate the early treatment process. The expert directly discusses a specific clinical scenario at [01:20] where a patient presents with textbook inflammatory symptoms but shows absolutely clear standard X-rays. This specific, highly deceptive clinical presentation is officially classified in the medical community as non-radiographic axial spondyloarthritis.
Despite the complete lack of visible bone damage on a basic X-ray film, these specific individuals are still dealing with a highly legitimate and deeply painful disease. The modern medical community now firmly recognizes that this non-radiographic phase is simply an earlier or slightly less structurally destructive form of the exact same autoimmune condition. Patients correctly placed in this diagnostic category experience the exact same debilitating morning stiffness and severe night pain as those with highly visible joint fusions.
Historically, chronic pain patients with perfectly clear X-rays were often quickly dismissed by doctors or incorrectly told their severe physical pain was merely psychological. The formal medical recognition of non-radiographic axial spondyloarthritis has completely revolutionized exactly how rheumatologists approach early-stage spine inflammation today. It properly validates the patient's intense physical suffering and immediately opens the clinical door for highly proper medical treatment long before the spinal bones actually begin to fuse.
Why Women Frequently Experience Non-Radiographic Symptoms
Extensive clinical data firmly indicates that the non-radiographic variant of this spinal disease presents with highly unique demographic patterns. The medical specialist specifically notes at [01:43] that this specific diagnostic template is particularly common among affected female patients. Women highly tend to experience the severe inflammatory symptoms constantly without developing the rapid, visible skeletal bone fusions typically seen in male rheumatology patients.
Because historical medical textbooks and early research primarily focused on the rapid spinal fusions seen predominantly in men, women were frequently severely underdiagnosed. Their completely clear standard X-rays led many primary care physicians to incorrectly rule out systemic joint inflammation entirely, leaving them without proper care. Modern, highly updated diagnostic criteria now fully account for these crucial gender differences, ensuring female patients rapidly receive the necessary specialized medical treatments.
It is highly critical for patients to understand that the non-radiographic phase is not always a permanent, stable state for the body. Over a period of several painful years, completely untreated non-radiographic inflammation can eventually naturally progress to highly visible structural damage on future X-rays. Continuous medical monitoring is absolutely essential to effectively track the disease's silent progression and proactively adjust therapeutic strategies before permanent skeletal damage solidifies.
The Danger of Misdiagnosing Spinal Inflammation as Fibromyalgia
The clinical diagnostic overlap between various chronic pain conditions frequently leads to highly frustrating medical dead ends for suffering patients. As strictly highlighted at [02:07], patients with perfectly clean X-rays and negative genetic blood tests are often wrongly diagnosed with generalized fibromyalgia. This severe medical misdiagnosis occurs primarily because general practitioners cannot easily find a definitive structural or genetic cause for the patient's severe widespread physical pain.
Fibromyalgia is generally classified as a central nervous system disorder that artificially amplifies pain signals, but it completely lacks actual joint inflammation or physical tissue damage. Treating a patient who actually has active spinal inflammation with standard fibromyalgia nerve medications will not ever stop the underlying aggressive autoimmune attack. The totally unchecked cellular inflammation will simply continue to silently damage the sacroiliac joints while the patient dutifully takes entirely ineffective nerve pain medications.
Being confidently told by a doctor that "there is nothing physically wrong with you" is incredibly discouraging for patients experiencing very real, deeply debilitating night pain. It practically forces many individuals to simply endure their worsening physical symptoms without any realistic hope for targeted, effective medical relief. Expert rheumatologists strongly urge anyone previously diagnosed with fibromyalgia who also regularly experiences severe morning stiffness to immediately seek a second specialized expert opinion.
Re-evaluating Normal Test Results in Chronic Pain Patients
A completely negative result on a specific genetic blood test does not ever automatically rule out a serious autoimmune spine condition entirely. While the HLA-B27 gene marker is strongly associated with the disease, a highly significant percentage of verified patients test completely negative for it. Relying far too heavily on a single basic blood test often naturally leads inexperienced doctors to mistakenly dismiss a highly probable, visually obvious clinical diagnosis.
Chronic pain patients must strictly and aggressively advocate for their own health if their current medical treatment plan consistently fails to provide meaningful daily pain relief. Directly requesting an advanced, high-resolution pelvic MRI is almost always the necessary next clinical step to reliably uncover hidden deep tissue inflammation that basic X-rays and blood work completely missed. Highly specialized rheumatology centers are fully equipped to expertly look far beyond basic laboratory test results and properly analyze the entire clinical physical picture accurately.
Promptly correcting a severe medical misdiagnosis completely alters the long-term trajectory of a patient's overall health and functional daily mobility. Transitioning rapidly from entirely ineffective nerve medications to highly targeted, modern biologic therapies can predictably yield highly dramatic physical improvements in daily function within just a few short weeks. Highly accurate medical re-evaluation is the absolute key to properly reclaiming a fully normal, highly active daily life completely free from severe chronic back pain.
Why Patients Choose Advanced Ankylosing Spondylitis Treatment in Turkey
The global landscape of specialized medical care is rapidly shifting, and modern Turkey has firmly positioned itself at the absolute forefront of advanced rheumatology. Patients from all around the globe are specifically traveling to modern Turkish medical centers to directly access highly comprehensive and incredibly accurate diagnostic services. The healthcare system there perfectly combines cutting-edge imaging technology with highly experienced medical specialists who focus entirely on treating complex autoimmune disorders.
One of the absolute primary draws for international travelers is the immediate, unrestricted access to highly modern biologic medications and targeted disease-modifying immune therapies. In many standard Western countries, suffering patients face highly strict insurance hurdles and incredibly long hospital waiting lists before they can safely receive these advanced infusion treatments. Turkish private hospitals reliably provide a highly streamlined medical process, readily allowing international patients to begin their specialized medication protocols without unnecessary, painful bureaucratic delays.
The highly multidisciplinary approach strictly utilized in top Turkish clinics ensures that every single aspect of the patient's physical condition is thoroughly and professionally addressed. Expert rheumatologists work directly alongside highly trained physical therapists, clinical dietitians, and dedicated pain management specialists to carefully create a totally holistic treatment plan. This highly collaborative medical environment consistently produces vastly superior long-term health outcomes compared to the highly fragmented standard care structures found in other global regions.
Combining Biologic Medications with Physical Therapy
Relying on standard medication alone is almost rarely enough to fully manage the highly complex physical limitations directly caused by chronic, severe spine inflammation. Highly comprehensive treatment programs heavily emphasize the strict integration of continuous, highly targeted physical rehabilitation perfectly alongside biological immune suppressants. The advanced medication effectively halts the active internal cellular inflammation, while expert physical therapy actively rebuilds the rapidly lost joint flexibility and surrounding core muscle strength.
Premium Turkish medical rehabilitation centers are highly equipped with highly advanced hydrotherapy healing pools and highly specialized spinal stretching physical equipment. Guided aquatic physical therapy is particularly medically beneficial simply because the natural buoyancy of the warm water completely removes the heavy physical load from the highly inflamed sacroiliac joints. Suffering patients can comfortably perform highly deep stretching physical exercises in the water that would be far too intensely painful to ever attempt on solid ground.
Highly customized daily physical exercise routines are meticulously designed by experts to vastly improve overall lung capacity and strictly maintain proper, healthy upright posture. Because the progressive disease frequently causes the entire human spine to slowly curve forward, dedicated physical therapists focus heavily on aggressive back extension structural exercises. Fully empowering patients with these specific physical therapy techniques ensures they can actively protect their natural spinal alignment long after they successfully return to their home country.
Navigating the Cost of Rheumatology Care in Turkey
Properly understanding the overall financial aspects of actively managing a highly lifelong autoimmune condition is absolutely crucial for international patients seeking total quality care. Advanced ankylosing spondylitis treatment in Turkey is highly globally renowned for being incredibly cost-effective without ever compromising slightly on strict medical excellence. The total overall out-of-pocket expenses for extensive MRI diagnostics, multiple specialist clinical consultations, and ongoing physical therapy sessions are significantly lower than in the United States or Western Europe.
This remarkable medical affordability directly extends to the long-term continuous procurement of highly advanced biologic medications and ongoing expert medical supervision. Many international medical patients quickly find that heavily factoring in the total cost of international travel and comfortable accommodation still readily results in massive overall financial medical savings. Highly transparent medical pricing models strictly utilized at top Turkish medical facilities readily allow patients to effectively plan their total healthcare budget without constantly fearing hidden hospital fees.
Looking far beyond just the immediate financial travel savings, directly investing in highly accurate early medical diagnosis pays massive, lifelong physical dividends in the long run. Actively preventing fully irreversible spinal bone fusions entirely eliminates the future medical need for highly complex, highly dangerous, and wildly expensive corrective orthopedic spine surgeries. Properly securing expert medical intervention highly early fundamentally protects the patient's future personal earning capacity and heavily preserves their overall independent, pain-free daily lifestyle.
Long-Term Rehabilitation and Lifestyle Adjustments
Successfully managing this highly specific autoimmune joint condition requires a highly permanent personal commitment to highly specific dietary and functional lifestyle modifications. Expert clinical nutritionists based in Turkey often directly help international patients design highly specialized, strictly anti-inflammatory diets to naturally support their advanced medical treatments. Strictly reducing the daily intake of highly processed foods and heavily increasing natural Omega-3 fatty acids can significantly reliably lower the human body's overall systemic inflammatory physical burden.
Making highly strict ergonomic physical adjustments in the daily workplace and at home is absolutely essential for strongly preventing highly unnecessary physical strain on the vulnerable spine. Diagnosed patients are heavily medically advised to immediately invest in highly supportive orthopedic mattresses and specialized ergonomic office chairs that actively promote a strictly neutral spinal posture. Implementing these highly simple physical changes to the daily physical environment can drastically and reliably reduce the overall frequency of highly severe mechanical pain flare-ups.
The ultimate medical goal of actively seeking highly comprehensive specialized care is to totally transition the suffering patient from a strict state of chronic suffering to highly active daily disease management. With the absolute right perfect combination of expert medical diagnostic guidance, highly advanced biologic therapies, and strict personal dedication, patients can rapidly achieve long-lasting physical remission. Taking absolute total personal control of the entire medical treatment journey readily allows affected individuals to finally live highly full, highly physically active lives completely unhindered by severe joint inflammation.
Start Your Journey to a Pain-Free Life Today
Don't let chronic back pain dictate your future. Connect with top rheumatology experts in Turkey for a highly accurate diagnosis and a customized treatment plan designed specifically for you.
Get Free QuoteView Full Video Transcript
00:00 Ankilozan spondilit genellikle sakroiliak ekleminde ba?lar.
00:05 Sakroiliak, yani kuyruk sokumu le?en kemi?i aras?ndaki eklem sakroiliak ile ba?lar.
00:11 Ve bu iltihap daha sonra yukar? do?ru omurgaya ç?kar.
00:14 Genellikle ankilozan spondilit için hep enflamatuvar bel a?r?s?ndan bahsederiz.
00:19 Biz bunu alt bel de dahil ederiz.
00:21 Enflamatuvar bel a?r?s?nda hasta, fazla istirahatle daha kötü olur.
00:25 Yani istirahatle a?r?lar? artar ve hareket etti?inde azal?r a?r?lar?.
00:31 Dolay?s?yla bu hastalarda genellikle gece a?r?s? olur.
00:34 Özellikle gecenin ikinci yar?s?, sabaha kar?? hastalarda ya bel tutuklu?u ya da a?r? söz konusudur.
00:42 Bu bulgular özellikle 45 ya? alt? birisinde ve 3 aydan fazla devam ederse bize ankilozan spondiliti dü?ündürülür.
00:51 Ankilozan spondilit tan?s?n? do?rulamak için, enflamatuvar bel a?r?lar? e?li?inde ayr?ca bir röntgen bak?l?r.
00:59 Bu röntgenlerde de?i?iklikler görürsek, yani iltihapl? romatizmaya ba?l?, özellikle sakroiliak ekleminde tan?y? oradan do?rulayabiliriz.
01:08 Ancak bazen hastada klasik ankilozan spondilit ?ikayetleri vard?r;
01:13 Enflamatuvar bel a?r?s?, sabah tutuklu?u,
01:16 ancak bu hastada röntgende bulgular yoktur.
01:20 Biz buna non-radyografik aksiyel spondiloartropati demekteyiz.
01:24 Bu hastalar da ankilozan spondilittir.
01:27 Non-radyografik aksiyel spondiloartropati, ankilozan spondilit hastalar? bizim için de çok önemlidir,
01:34 çünkü zamanla bu hastalar ankilozan spondilite geçebilir,
01:37 yani radyografik röntgende görünen veya MR'da görünen ankilozan spondilite de geçebilir.
01:43 Özellikle kad?nlarda biz bu ?ablonu görmekteyiz.
01:46 Bazen röntgende görünmüyor, non-radyografik.
01:49 Seneler sonra radyografik röntgende görünebilir.
01:52 Her ikisi de ankilozan spondilit diyor asl?nda.
01:56 Dolay?s?yla geçmi?te bir hasta klasik enflamatuvar bel a?r?s? olup,
02:01 ancak gen testi temiz ç?k?p veya röntgende görünmediyse
02:05 ve hastaya "sizde bir ?ey yok" deyip, "sizde sadece fibromiyalji vard?r" dendiyse,
02:10 bu hastan?n tekrar gözden geçirilmesi laz?m.
02:13 Çünkü bu hastalarda asl?nda ankilozan spondilit olabilir.




.png)
.png)

.png)






Share this listing