Short-Stem Total Hip Arthroplasty: The Future of Bone-Preserving Joint Replacement
Hip replacement surgery has long been considered one of the most successful surgical interventions of the 20th century. However, as the patient demographic shifts toward younger, more active individuals, the medical community has sought innovations that prioritize bone conservation and natural joint mechanics. Short-stem total hip arthroplasty represents a significant leap forward in this field, offering a less invasive alternative to traditional long-stem implants. By focusing on the upper femur, this technique allows surgeons to restore mobility while respecting the patient's unique anatomy.
In this featured presentation, Prof. Dr. Karl Philip Kutzner delves into the specific mechanical and clinical advantages of short-stem implants. Whether you are a patient exploring surgical options or a healthcare enthusiast curious about orthopedic trends, understanding why this "less is more" approach is gaining global traction is essential. Watch as we break down the science of bone preservation, the nuances of minimally invasive implantation, and the accelerated path to postoperative rehabilitation.
Video Chapters & Quick Navigation
Understanding Short-Stem Hip Arthroplasty
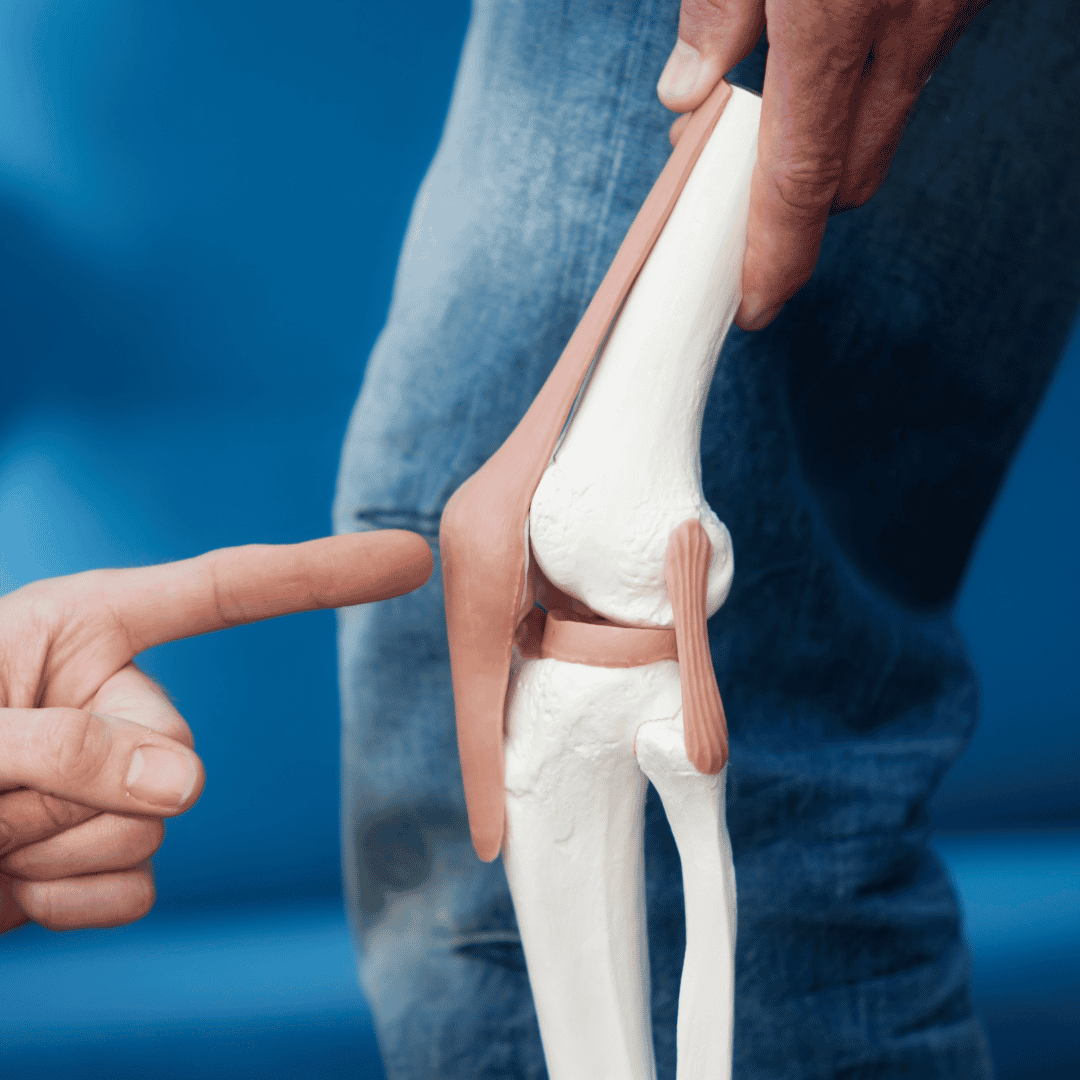
Traditional hip replacement stems are typically designed to extend deep into the femoral canal. This "diaphyseal anchoring" has worked for decades, but it requires significant removal of healthy bone marrow and cortical bone. As Prof. Dr. Kutzner explains at [00:13], a short stem is a specialized type of prosthesis characterized by its reduced length. Unlike traditional implants, the short stem is anchored primarily in the "metaphyseal" or upper region of the femur.
This design shift is not just about length; it is about how the bone carries weight. By anchoring higher up, the short stem mimics the way a natural hip transmits forces. This helps prevent "stress shielding," a common issue with longer stems where the bone becomes thin and weak because the metal implant is carrying all the load instead of the bone itself. The evolution toward short stems reflects a broader trend in orthopedics: moving from "aggressive" surgery to "anatomical" restoration.
Key Differences: Short vs. Traditional Stems
| Feature | Traditional Long Stem | Modern Short Stem |
|---|---|---|
| Anchoring Point | Deep Femoral Canal (Diaphysis) | Upper Femur (Metaphysis) |
| Bone Removal | Extensive removal of marrow/bone | Minimal removal; bone-preserving |
| Ideal Candidate | Elderly with lower bone density | Younger, active, high bone quality |
| Revision Ease | More complex due to bone loss | Easier; more original bone remains |
The Crucial Advantage of Bone Tissue Preservation
One of the most compelling arguments for short-stem implants is the preservation of native bone tissue [00:38]. This is particularly vital for patients in their 40s, 50s, or 60s who may eventually require a revision surgery decades down the line. Every hip implant has a lifespan, and when it needs to be replaced, having a healthy "stock" of original bone makes the second surgery much safer and more successful.
Because the short stem is less intrusive, the femoral neck is often partially preserved. This maintains the natural "offset" and "version" of the hip, which are the fancy medical terms for the geometry that allows your leg to swing and rotate comfortably. When we save bone, we save the structural integrity of the femur, ensuring that the patient remains a candidate for future medical advancements should the need arise.
Minimally Invasive Surgery and Surgical Efficiency
The smaller size of short-stem prostheses facilitates a less invasive surgical approach [00:52]. Surgeons can often use smaller incisions and muscle-sparing techniques, such as the Direct Anterior (DA) approach, more effectively with these implants. Since the implant itself is shorter, it requires less maneuvering through the soft tissues and muscles surrounding the hip joint.
This translates to several direct clinical benefits:
- Reduced Operation Time: Faster implantation means the patient is under anesthesia for a shorter duration.
- Decreased Blood Loss: By avoiding the deep femoral canal, there is often less intraoperative bleeding.
- Lower Risk of Infection: Shorter surgical times and smaller incisions are statistically linked to lower rates of postoperative infection.
Accelerated Recovery: Getting Back to Life Faster
The modern patient doesn't just want to walk; they want to hike, cycle, and return to work without a long, grueling recovery process. As highlighted at [01:03], patients receiving a short-stem hip often benefit from a significantly faster rehabilitation period. Because the surrounding muscles and tendons are better protected during surgery, the joint feels "stable" almost immediately.
Physiotherapy can often begin on the very day of surgery or the day after. The reduction in postoperative pain allows patients to mobilize sooner, which is the best defense against complications like deep vein thrombosis (DVT) or pneumonia. For those who value their independence and quality of life, the "fast-track" recovery associated with short-stem arthroplasty is a game-changer.
Respecting Natural Anatomy and Joint Kinematics
No two humans have the exact same hip geometry. One of the technical hurdles with traditional stems is that they sometimes force the patient's anatomy to fit the implant. Short stems, by contrast, are designed to adapt to the patient's natural femoral shape [01:14]. This results in better "kinematics"—the way the joint moves in three-dimensional space.
When the kinematics are natural, the "forgotten hip" phenomenon is more likely to occur. This is the ultimate goal of orthopedic surgery: a joint that the patient no longer thinks about because it feels like a part of their own body. Improved kinematics also mean less wear and tear on the prosthetic components themselves, potentially extending the life of the artificial joint.
Long-Term Stability and Dislocation Prevention
A primary concern with any hip replacement is the risk of dislocation. However, the unique anchoring and anatomical fit of the short stem actually enhance the stability of the joint [01:38]. By allowing for a more precise restoration of the hip's original center of rotation, the surrounding soft tissues and ligaments maintain their natural tension.
Data from long-term clinical registries have shown that short stems, when implanted by experienced surgeons, have exceptional survival rates. They provide a "tight fit" in the metaphyseal bone that promotes rapid osseointegration—where the bone grows directly onto the surface of the metal. This biological bond is what provides the rock-solid stability required for an active lifestyle.
Who Should Consider Short-Stem Hip Arthroplasty?
While the advantages are numerous, it is important to note that this procedure is not for everyone. Surgeons generally recommend short-stem implants for:
- Patients with good primary bone quality (Dorr Type A or B).
- Individuals under the age of 70 who lead active lifestyles.
- Patients with specific anatomical variations that make traditional stems difficult to fit.
- Those who prioritize a bone-conserving approach for potential future needs.
Ready to Restore Your Smile in Egypt?
PlacidWay Medical Tourism connects you with top-rated dental clinics in Egypt, offering world-class care at unbeatable prices. Let us handle the details while you focus on your new smile.
GET A FREE QUOTE









.png)


Share this listing