Understanding Laparoscopic Inguinal Hernia Surgery: A Complete Patient Guide
Living with chronic groin pain can entirely disrupt your daily life, turning simple activities like lifting groceries or exercising into agonizing tasks. For years, patients have delayed treatment due to the fear of long recovery times and painful incisions associated with traditional operations.
Today, advanced medical technology has revolutionized abdominal wall repair. Laparoscopic Inguinal Hernia Surgery offers a minimally invasive alternative that significantly reduces postoperative discomfort and accelerates recovery. Watch this patient testimonial to discover firsthand how modern surgical techniques are helping individuals reclaim their active lifestyles safely, efficiently, and with minimal downtime.
Video Chapters & Quick Navigation
The Physiology and Anatomy of an Inguinal Hernia
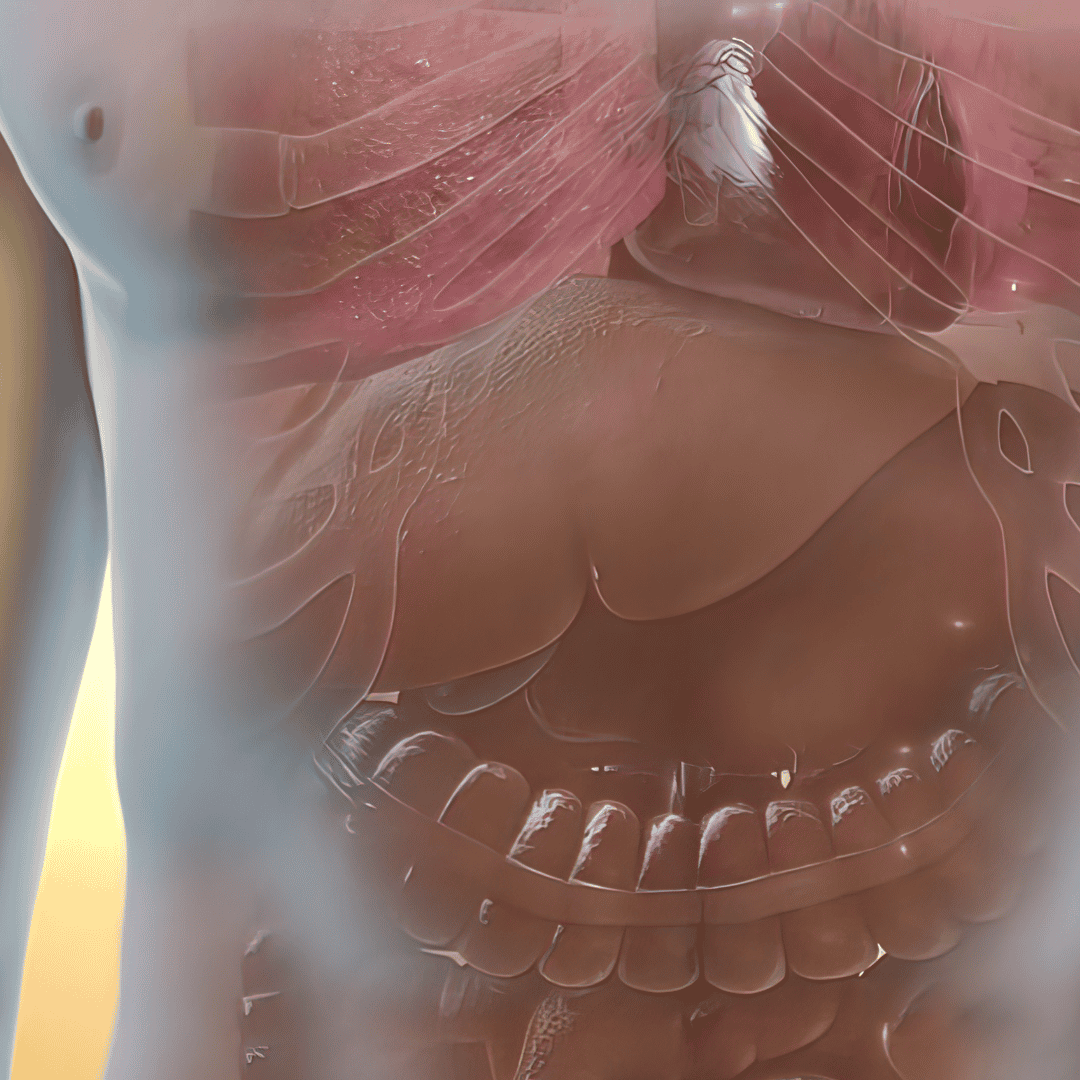
To fully appreciate the brilliance of modern laparoscopic solutions, it is crucial to first understand the structural failure that causes a hernia. An inguinal hernia occurs when soft tissue, typically part of the intestine or abdominal fat, protrudes through a weak spot or tear in the lower abdominal wall. This region, known as the inguinal canal, is a naturally vulnerable area in the human anatomy.
In men, the inguinal canal holds the spermatic cord, while in women, it contains the round ligament that supports the uterus. Because the male inguinal canal is naturally larger to accommodate the descent of testicles during fetal development, men are statistically far more likely to develop this specific type of hernia. However, women are not entirely immune, and the signs of an inguinal hernia can manifest unexpectedly regardless of gender.
Patients often first notice a distinct bulge in the pelvic or groin region that becomes more pronounced when standing, coughing, or straining. This physical protrusion is frequently accompanied by a dull, heavy ache or a sudden sharp burning sensation. If the protruding tissue becomes trapped or strangulated, it can cut off blood supply to the intestines, creating a life-threatening medical emergency that requires immediate surgical intervention.
Recognizing Early Warning Signs and Symptoms
Many individuals live with a minor abdominal wall defect for years before the symptoms become severe enough to disrupt their routine. It often starts as a vague feeling of pressure in the groin at the end of a long day of standing or heavy lifting. As the internal abdominal pressure pushes more tissue through the fascial defect, the symptoms rapidly escalate.
Understanding the signs of an inguinal hernia in men and women early on can prevent the need for emergency surgery. Symptoms that warrant an immediate consultation with a hernia specialist include persistent chronic groin pain, a bulge that cannot be pushed back into the abdomen while lying down flat, and sudden nausea or vomiting. Early detection provides patients with the luxury of scheduling an elective, minimally invasive repair before complications arise.
The Evolution of Treatment: Laparoscopic vs Open Hernia Repair
For decades, the standard protocol for repairing a groin hernia was traditional open surgery, often referred to as a Lichtenstein repair. This conventional technique requires the surgeon to make a significant incision directly over the hernia site, which can measure anywhere from three to six inches in length. The surgeon then manually pushes the protruding tissue back into place and sews a synthetic mesh over the weakened muscle to reinforce it.
While traditional open surgery remains a highly effective and safe method, it requires cutting through multiple layers of skin, fat, and healthy muscle tissue. This extensive tissue disruption inevitably leads to a more painful postoperative experience and a significantly longer rehabilitation period. Furthermore, open surgery carries a higher risk of chronic nerve entrapment, which can lead to lingering, long-term groin pain.
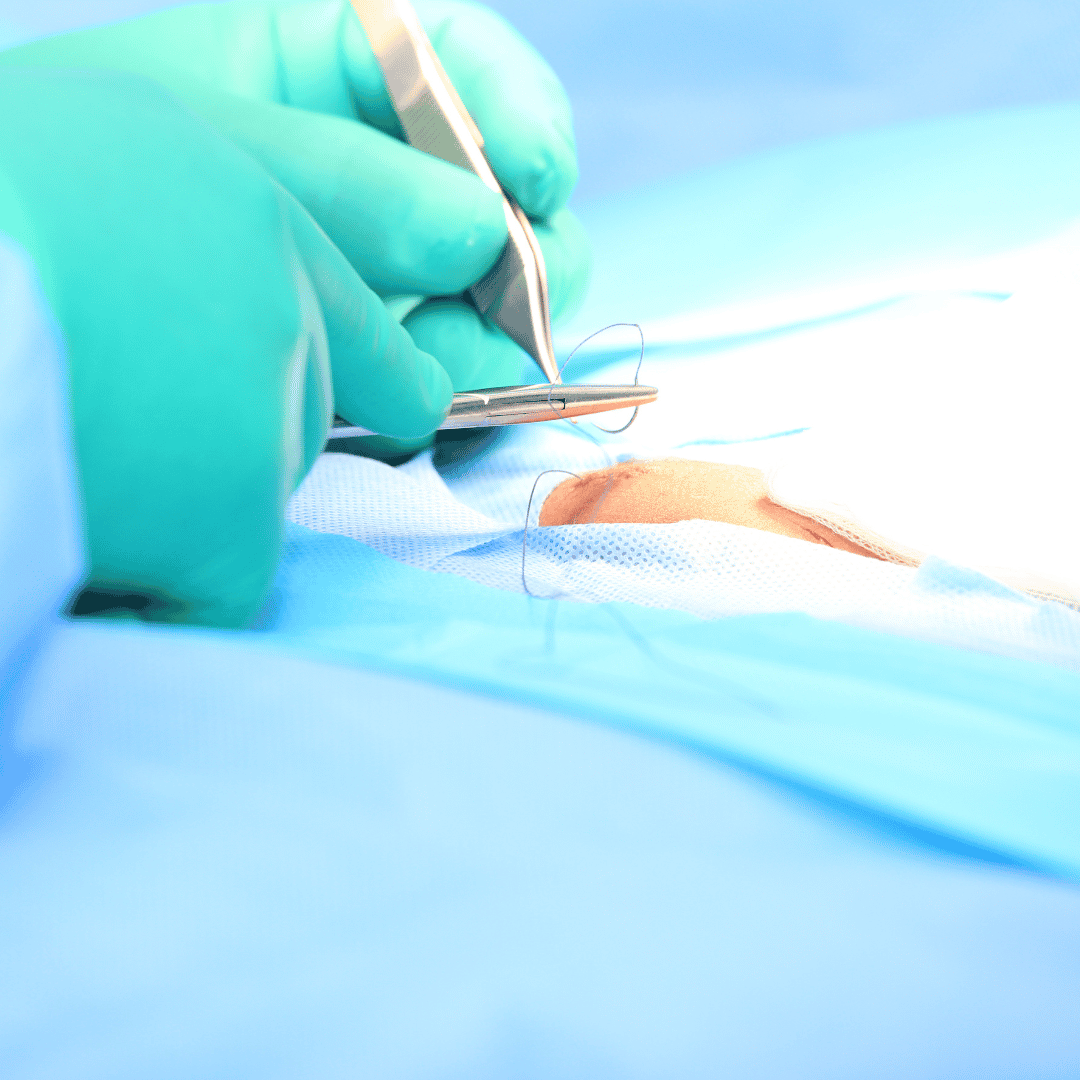
Conversely, a minimally invasive inguinal hernia repair completely changes the surgical approach. Instead of a large incision, the surgeon creates three tiny incisions, usually no larger than a centimeter each. Through these small portals, high-definition cameras and specialized elongated instruments are inserted to perform the entire repair from the inside out. This approach leaves the outer abdominal wall entirely intact, preserving muscle integrity.
A Clear Comparison of Surgical Methods
| Feature | Traditional Open Surgery | Laparoscopic Hernia Surgery |
|---|---|---|
| Incision Size | One large incision (3-6 inches) | Three small "keyhole" incisions |
| Muscle Damage | Requires cutting through muscle layers | Muscles are separated, not cut |
| Bilateral Repair | Requires two separate large incisions | Both sides repaired through same 3 tiny incisions |
| Return to Work | Typically 4 to 6 weeks | Typically 1 to 2 weeks |
| Post-Op Pain | Moderate to severe in the first week | Mild, easily managed with basic analgesics |
Why Choose Minimally Invasive Laparoscopic Solutions?
When reviewing your options with a general surgeon, the benefits of laparoscopic techniques become incredibly clear, particularly for specific patient demographics. One of the most significant advantages is seen in patients suffering from bilateral hernias—meaning they have hernias on both the left and right sides of their groin.
In traditional open surgery, a bilateral repair necessitates two entirely separate, painful incisions. However, with advanced laparoscopic solutions, the surgeon can access and repair both sides of the pelvis using the exact same three tiny keyhole incisions. This dramatically reduces operative trauma and prevents the patient from having to endure double the recovery pain.
Furthermore, minimally invasive methods offer superior visualization of the pelvic floor anatomy. High-definition surgical monitors provide surgeons with a magnified, highly illuminated view of the defect from behind the abdominal wall. This allows for precise placement of the inguinal mesh repair, ensuring a tension-free fix that significantly lowers the lifetime risk of hernia recurrence.
Deep Dive into the Surgical Procedure: How It Works
Entering an operating room can be incredibly intimidating, but understanding the exact mechanics of the procedure can alleviate much of this preoperative anxiety. Laparoscopic inguinal hernia surgery is performed under general anesthesia, ensuring that the patient is entirely asleep and comfortably unaware throughout the entire duration of the procedure.
Once the patient is safely anesthetized, the surgical team gently inflates the abdomen with harmless carbon dioxide gas. This inflation creates a spacious working dome, lifting the abdominal wall away from the internal organs to give the surgeon ample room to maneuver. There are two primary techniques utilized in this field: TAPP (Transabdominal Preperitoneal) and TEP (Totally Extraperitoneal).
The TAPP and TEP Methodologies
- The TAPP Approach: The surgeon enters the main peritoneal cavity (where the organs reside) to visually inspect the hernia before peeling back the peritoneum (the inner abdominal lining) to place the surgical mesh.
- The TEP Approach: This highly advanced technique avoids entering the main abdominal cavity entirely. The surgeon creates a space between the muscle and the inner lining to deploy the mesh, reducing the risk of internal organ injury and postoperative adhesions.
Regardless of the specific technique chosen, the core objective remains the same. The herniated tissue is carefully coaxed back into its proper anatomical position. A highly durable, sterile piece of synthetic mesh is then unrolled over the weakened fascial defect like a patch on a tire. Over the following weeks, the body's natural healing process will weave new tissue through the pores of this mesh, creating a permanent, reinforced biological barrier.
Patient Testimonials: Real Experiences with Laparoscopic Hernia Repair
Medical literature and surgical statistics are vital, but there is no substitute for hearing directly from those who have undergone the knife. The emotional and physical toll of living with a hernia is heavy. As highlighted in the video at , patients often express deep frustration over their inability to participate in sports, play with their children, or simply perform their occupational duties without fear of an agonizing flare-up.
Testimonials frequently focus on the stark contrast between the intense fear of surgery and the surprising ease of the reality. At in the video, we hear the patient describe the immediate relief felt upon waking up. The persistent, heavy pressure in the groin was instantly gone, replaced only by mild surgical soreness. This rapid transition from chronic suffering to immediate resolution is the hallmark of modern laparoscopic techniques.
Another profound point raised in patient testimonials revolves around the speed of discharge. Because the procedure is so minimally invasive, it is almost exclusively performed on an outpatient basis. As noted around , patients are typically walking the halls of the surgical center within hours of waking up and are cleared to return to the comfort of their own homes on the exact same day.
Navigating Laparoscopic Hernia Surgery Recovery Time
The phrase "surgery recovery" usually conjures images of prolonged bed rest and debilitating pain, but the laparoscopic hernia surgery recovery time is a remarkably swift trajectory. However, it is essential to follow clinical guidelines strictly to allow the internal mesh to properly fuse with your natural tissues. Pushing yourself too hard, too fast, can jeopardize the repair.
During the first 24 to 48 hours, patients will experience mild to moderate soreness around the three small incision sites, as well as some temporary shoulder pain. This shoulder pain is actually referred pain caused by the residual carbon dioxide gas used to inflate the abdomen pressing against the diaphragm. Walking frequently but gently around the house is highly encouraged during this phase to help the body safely absorb and expel this gas.
The Weekly Breakdown of Resuming Normal Life
By the end of the first week, the vast majority of patients no longer require any prescription pain medication, transitioning completely to over-the-counter anti-inflammatories. Desk workers and those with sedentary occupations are often cleared to return to their jobs at this point. The tiny keyhole incisions will begin to form small, clean scabs, and bruising around the groin area will start to fade.
Weeks two through four mark a significant return to normalcy. Patients can begin reintroducing light cardiovascular exercises, such as brisk walking, stationary cycling, and gentle swimming. However, it is absolutely critical during this period to avoid lifting anything heavier than 15 pounds. The internal mesh is still in the active phase of biological integration, and sudden spikes in intra-abdominal pressure can cause the tacks holding the mesh to fail.
Once the six-week milestone is reached, most surgeons will officially discharge the patient from all physical restrictions. The tissue ingrowth is completely solidified. At this stage, patients can confidently return to high-impact activities, heavy weightlifting, and strenuous manual labor, completely free of the chronic groin pain that once held them back.
Risks, Complications, and Long-Term Success Rates
While minimally invasive inguinal hernia repair is overwhelmingly safe and carries a high success rate, it is vital to approach any surgical procedure with a comprehensive understanding of potential risks. The most common minor complications are localized seromas or hematomas—small collections of fluid or blood that accumulate in the space where the hernia used to be. These typically resolve independently as the body naturally reabsorbs the fluid.
Urinary retention is another temporary, post-surgical hurdle that some patients experience immediately following the operation. The use of general anesthesia, combined with swelling in the pelvic region, can temporarily stun the bladder. Medical staff will closely monitor urinary output before allowing a patient to go home to ensure standard bladder function has fully returned.
When looking at the long-term outlook, laparoscopic techniques boast incredible success. The rate of hernia recurrence following a properly executed laparoscopic mesh repair is exceptionally low, typically hovering around 1% to 2%. Furthermore, because the mesh is placed behind the abdominal defect rather than sewn on top of it, the natural outward pressure of the abdomen actually helps hold the mesh firmly in place, utilizing the body's own biomechanics to secure the repair.
Cost Analysis: Planning Your Laparoscopic Inguinal Hernia Surgery
One of the final, yet most significant hurdles patients face is the financial aspect of elective surgery. A bilateral inguinal hernia surgery cost in the United States or Western Europe can easily exceed tens of thousands of dollars, particularly for underinsured patients or those dealing with high-deductible healthcare plans. The facility fees, anesthesia costs, and the specialized laparoscopic equipment all contribute to a hefty final bill.
Because of this financial barrier, an increasing number of patients are turning to global medical tourism. World-class medical facilities across Latin America, Eastern Europe, and Asia offer access to board-certified, internationally trained general surgeons utilizing the exact same premium synthetic meshes and high-definition laparoscopic towers as top-tier Western hospitals.
By exploring medical travel options, patients can often bundle their pre-op consultations, the surgery itself, facility fees, and even post-operative hotel stays into a single, affordable, transparent package. This democratizes access to advanced healthcare, ensuring that no patient is forced to endure chronic groin pain simply because local healthcare costs are prohibitively expensive.
Preparing for Your Hernia Consultation
Taking the first step toward living a pain-free life begins with a thorough surgical consultation. When you meet with a specialized hernia surgeon, come prepared with a detailed list of your symptoms, a timeline of when you first noticed the bulge, and notes regarding which daily activities cause you the most discomfort. Honesty about your lifestyle and physical demands is crucial for tailoring the surgical approach.
Do not hesitate to ask highly specific questions during your appointment. Inquire about the surgeon's personal experience with TEP versus TAPP techniques. Ask about the specific brand and material of the surgical mesh they intend to use, and request a detailed overview of their personal complication and recurrence rates. A confident, skilled surgeon will welcome these questions and provide transparent, reassuring answers.
Ultimately, a laparoscopic hernia surgery is more than just a medical procedure; it is a profound restoration of your quality of life. The modern advancements in surgical precision have minimized the risks and recovery barriers that once kept patients suffering in silence. By educating yourself on the anatomy, the surgical methodologies, and the recovery expectations, you empower yourself to make the best possible decision for your long-term health and wellness.
Ready to Reclaim Your Active Lifestyle?
Stop letting chronic groin pain dictate what you can and cannot do. PlacidWay connects you with globally accredited hospitals and board-certified surgeons offering highly affordable, minimally invasive laparoscopic hernia repairs.
REQUEST YOUR FREE MEDICAL QUOTE

.png)










Share this listing